
Loose Dental Implant in Chevy Chase, MD
Loose implants in Chevy Chase often signal peri-implantitis, a bacterial infection around the implant. Dr. Marlin treats bone loss and infection. Call now.
Loose Dental Implant Due to Peri-Implantitis in Chevy Chase, MD
A loose implant often whispers a warning that many patients miss until the problem advances. That warning is peri-implantitis: a bacterial infection attacking the bone and soft tissues supporting your implant. Unlike a simple abutment screw that backs out, peri-implantitis represents an ongoing biological threat that worsens without intervention. At Elite Prosthetic Dentistry, we detect and treat peri-implantitis aggressively, because early action often saves the implant while advanced cases demand extraction and replacement.
Understanding Peri-Implantitis: The Silent Implant Destroyer
Peri-implantitis is insidious. It starts quietly, often without pain or obvious symptoms. You might notice slight mobility in your implant, or your general dentist might spot bone loss on a routine radiograph. By the time patients feel significant discomfort or swelling, the problem is often advanced.
The Bacterial Biofilm Problem
Your mouth contains hundreds of bacterial species. Under normal conditions, your immune system and hygiene practices keep them in balance. But around dental implants, conditions can shift dangerously. Biofilm, the sticky bacterial community that forms on all tooth and implant surfaces, can accumulate more aggressively around implants than around natural teeth.
Natural teeth have a periodontal ligament, a fibrous attachment that provides a vascular blood supply to the tooth root and surrounding tissues. This blood supply helps fight infection. Dental implants lack this ligament. They have only direct bone-to-titanium contact. This anatomical difference is crucial. When bacteria breach the tissue barrier around an implant, the implant’s defenses are weaker than those of a natural tooth, so infection can advance faster and more destructively.
How the Infection Takes Hold
Peri-implantitis typically begins around the implant shoulder, the junction where the implant emerges from bone and transitions to soft tissue. If this area becomes contaminated with aggressive bacteria, the infection can spread along the implant surface. The bacteria produce toxins that trigger the body’s inflammatory response, which unfortunately damages bone as part of the immune reaction.
This is the critical concept: your own immune system, fighting the bacteria, causes bone loss. The bacteria themselves don’t eat bone like a cavity eats tooth structure. Instead, they trigger inflammation, and the inflammatory response includes bone destruction.
Risk Factors That Increase Susceptibility
Some patients are inherently more susceptible to peri-implantitis. We assess these factors during your evaluation.
Smoking dramatically increases peri-implantitis risk and is a key risk factor before implant placement. Cigarette smoke impairs healing and immune function around implants. Smokers with implants have significantly higher infection rates than non-smokers.
Diabetes, particularly if uncontrolled, slows healing and impairs the immune response to oral bacteria. Diabetic patients require more aggressive preventive measures around implants and benefit from comprehensive monitoring.
Poor oral hygiene creates an environment where biofilm accumulates unchecked. Patients who struggle with home care face higher peri-implantitis risk and may benefit from water flosser guidance and home care optimization.
Genetic factors play a role. Some individuals’ immune systems respond more aggressively to even modest bacterial challenges. This genetic variation in immune responsiveness can predispose certain patients to peri-implantitis.
History of periodontal disease indicates a susceptibility to bacterial challenges. If you had periodontal disease around natural teeth, you’re at higher risk for peri-implantitis around implants. Understanding bone loss patterns helps us manage your implant risk.
Certain medications that reduce saliva flow increase peri-implantitis risk. Saliva has antimicrobial properties and helps wash away bacteria.
Implants placed too close to adjacent natural teeth create spaces where bacteria accumulate. Poor surgical positioning increases infection risk.
Smoking, diabetes, poor hygiene, and genetic predisposition create a perfect storm for peri-implantitis. We discuss your specific risk profile and adjust prevention strategies accordingly.
How Peri-Implantitis Causes Implant Loosening
The connection between peri-implantitis and a loose implant is direct and mechanical.
The Bone Loss Cascade
Bone loss is the defining characteristic of peri-implantitis. As bacteria trigger inflammation, osteoclasts (bone-destroying cells) activate and remove bone tissue faster than osteoblasts (bone-building cells) can replace it. This net loss of bone height and volume reduces the contact area between the implant fixture and the surrounding bone.
An implant is stable because bone fully surrounds it and resists movement. As bone height decreases, the implant loses its anchors. Imagine a fence post set 24 inches deep versus 6 inches deep; the deeper post resists lateral movement far better. The same principle applies to dental implants.
Progressive Mobility
In early peri-implantitis, bone loss might be visible on radiographs but you may not feel any mobility. As the infection continues and bone loss progresses, enough bone is lost that the implant becomes perceptible loose. You might notice movement when you press on the crown with your tongue or finger. Eventually, the implant becomes visibly mobile.
This progression is why early detection is critical. We want to catch peri-implantitis before significant bone loss occurs, ideally at the radiographic stage before mobility develops.
The Inflammatory Exudate
Beyond bone loss, peri-implantitis produces fluid (exudate) around the implant. This inflammatory fluid reduces the effectiveness of bone-to-implant contact. Even if the bone volume seems adequate on imaging, the inflammatory compromise means the implant isn’t anchored as well as it should be. Treating the infection and reducing inflammation often improves stability even before new bone forms.
Diagnostic Approach to Peri-Implantitis
Our evaluation protocol is designed to catch peri-implantitis early and assess its severity accurately.
Clinical Examination Signs
We look for several clinical indicators. Redness and swelling around the implant gum line suggest active inflammation. Bleeding or pus when we gently probe around the implant indicates active infection. Mobility of the implant crown or fixture when we test it clinically confirms what radiographs suggest.
Radiographic Findings
Radiographs show bone levels around the implant. We compare current images to previous ones if available. Bone loss around an implant that was stable for years is a hallmark of peri-implantitis. We assess how much bone has been lost and how rapidly it’s being lost. Fast progression indicates more aggressive disease.
Probing Depth Measurement
Unlike natural teeth where we measure sulcus depth, we assess pocket depth around implants. A depth greater than 4 millimeters around an implant suggests peri-implantitis, particularly if there’s bleeding with probing. Deep pockets trap bacteria and make home care impossible.
Suppuration Assessment
Suppuration is the presence of pus. We check whether pus can be expressed from the tissues around the implant. The presence of suppuration indicates active, symptomatic infection.
Medical and Behavioral History
We ask detailed questions about your habits, medical conditions, and medications. Smoking, diabetes control, oral hygiene practices, and recent illness all inform our assessment.
Treatment Protocols for Peri-Implantitis
Treatment intensity depends on disease severity. We pursue implant salvage aggressively but understand when extraction becomes the better choice.
Non-Surgical Management Phase
Early peri-implantitis and mild cases often respond to aggressive non-surgical therapy.
Biofilm Removal
We perform thorough mechanical removal of biofilm from the implant surface and surrounding soft tissues. This is deeper and more aggressive than standard prophylaxis. We use specialized instruments that remove biofilm without damaging the implant surface.
Antimicrobial Therapy
We might recommend antimicrobial rinses, such as chlorhexidine, to suppress bacterial growth while tissues heal. Some patients use these temporarily at home after professional cleaning.
Antibiotic Prescription
For active infection with significant bone loss, we prescribe systemic antibiotics. Amoxicillin combined with metronidazole is effective against the polymicrobial anaerobic infections common in peri-implantitis. We culture when possible to tailor antibiotic selection.
Hygiene Optimization
We discuss home care intensively. Patients with peri-implantitis require immaculate hygiene. We recommend specific devices like water flossers or specialized implant brushes. We teach gentle but thorough cleaning to avoid damaging tissues while effectively removing biofilm.
Smoking Cessation
If you smoke, this is the critical intervention. Smoking’s detrimental effect on implant infection is so significant that some oral surgeons consider it a relative contraindication to implant therapy. We discuss smoking cessation resources and strongly encourage participation.
Medical Optimization
If you’re diabetic, achieving better blood sugar control improves implant healing. If you’re taking medications that reduce saliva, we explore alternatives with your physician.
Surgical Management Phase
If non-surgical management fails after 4-6 weeks, or if disease is advanced at presentation, surgical therapy becomes necessary.
Access Flap Surgery
We create an incision to access the bone and implant surfaces. This allows us to remove biofilm, calculus, and damaged tissue more thoroughly than non-surgical approaches permit.
Implantoplasty
If the implant surface itself is compromised by biofilm colonization, we smooth and polish the exposed implant surface. A smoother surface is less colonized by bacteria.
Bone Regeneration Procedures
For sites with contained bone defects (where the defect is surrounded by bone walls), we might place bone graft material to regenerate lost bone. This improves implant support and can re-stabilize the implant.
Guided Bone Regeneration
We sometimes use barrier membranes to protect graft material and direct bone healing. This technique can improve the amount of bone that regenerates.
Soft Tissue Graft
If the infection has destroyed a significant amount of soft tissue, a graft from another area in your mouth can restore tissue volume and support.
When Extraction Becomes the Right Choice
Sometimes, despite aggressive treatment, peri-implantitis cannot be controlled and the implant must be removed.
Indicators that extraction is appropriate include: bone loss beyond 50 percent of the implant length, implant mobility that doesn’t improve with treatment, radiographic evidence of continued bone loss despite intervention, or patient preference to start fresh with replacement rather than commit to long-term management.
Removal of a severely compromised implant often provides relief. The infection source is eliminated, and we can plan for replacement implant therapy or alternative restorations after bone healing.
Post-Treatment Management and Prevention
Once peri-implantitis is addressed, whether through non-surgical or surgical means, vigilant maintenance prevents recurrence.
Professional Visits
We schedule more frequent follow-up appointments than routine maintenance. During the first year after peri-implantitis treatment, we typically see you every 3 months instead of 6 months. This allows us to monitor for any signs of recurrence and reinforce hygiene.
Imaging Schedule
We take radiographs more frequently to monitor bone levels. If bone remains stable, we can lengthen the interval between imaging. If any rebound is noted, we intensify treatment.
Home Care Regimen
Patients with a history of peri-implantitis should use a water flosser daily around the implant area. A soft brush with gentle technique removes plaque without damaging tissues. Some patients benefit from antimicrobial rinses used indefinitely, not just during active treatment.
Risk Factor Management
If you smoke, staying quit is essential. If you’re diabetic, maintaining good control directly impacts implant health. If you have a history of periodontal disease, excellent hygiene habits protect both remaining natural teeth and implants.
Chevy Chase and Implant Health Maintenance
Chevy Chase residents tend to be engaged with their healthcare and willing to commit to maintenance. This mindset is ideal for implant patients with a peri-implantitis history. We work with patients who understand that implants, while not prone to decay, are still living in a living system and require active care and monitoring.
Our proximity to Chevy Chase, just 3 minutes away, means that follow-up appointments are convenient. This proximity removes logistical barriers to the frequent monitoring that post-peri-implantitis implants require.
Advanced Diagnostics We Offer
Beyond standard radiography, we employ several advanced diagnostic techniques that improve our ability to detect and monitor peri-implantitis.
Cone Beam Computed Tomography (CBCT)
3D imaging reveals bone loss patterns that standard radiographs might miss. CBCT shows us the severity and extent of bone loss in three dimensions, informing surgical planning if therapy is needed.
Sulcus Fluid Analysis
In research settings and some advanced practices, analysis of the fluid around the implant can indicate the presence of specific bacterial or inflammatory markers. While not routine, this analysis can guide treatment in complex cases.
Patient Education Through Imaging
We show you your radiographs and explain what we see. Many patients become more motivated to commit to excellent hygiene once they visualize bone loss. Seeing improvement on follow-up radiographs reinforces the value of your commitment.
Why Choose Elite Prosthetic Dentistry for Peri-Implantitis
Dr. Marlin’s Master of Science degree in Prosthodontics includes advanced training in implant complications and management. He understands peri-implantitis at both the basic biological level and the clinical treatment level.
Our in-house laboratory means we can fabricate implant components and temporary restorations quickly if your treatment requires implant surface management or repositioning. We don’t wait for external labs during critical treatment phases.
We maintain relationships with oral surgeons who specialize in advanced bone grafting and regeneration. When your case requires surgical expertise beyond prosthodontics, we coordinate care and ensure seamless treatment.
Related Conditions and Associated Services
Many patients with peri-implantitis benefit from understanding related service areas we provide. Dental implant bone loss is the hallmark of peri-implantitis, and understanding this process helps patients commit to the prevention and monitoring regimen necessary after treatment.
Repairing failing implants often incorporates peri-implantitis management as part of a broader salvage strategy. Failed implant integration sometimes manifests similarly to peri-implantitis but requires a different treatment approach.
Bone grafting is frequently part of surgical peri-implantitis management to regenerate lost bone volume. For Chevy Chase patients, we provide dental implants, bone grafting in Chevy Chase, implant repair in Chevy Chase, full mouth reconstruction in Chevy Chase, implant denture repair in Chevy Chase, and sedation dentistry in Chevy Chase.
If you’re considering future implants or implant replacement, precision implant placement is essential. Proper positioning reduces peri-implantitis risk significantly.
Prosthodontist in Chevy Chase provides comprehensive context on our services. Second opinion dentistry is appropriate if you’ve received a peri-implantitis diagnosis elsewhere and want confirmation.
Scheduling Your Evaluation
If you suspect peri-implantitis or have a loose implant with any signs of infection, urgent evaluation is warranted. Contact us to request an appointment. We can often accommodate urgent cases within 1-2 days.
Read more about Dr. Marlin’s approach to complex implant cases and his credentials.
Peri-implantitis is serious, but early detection and aggressive treatment save implants routinely. Early action transforms a loose, infected implant into a stable, functional restoration. Let us help you protect your implant investment.
Frequently Asked Questions
What exactly is peri-implantitis and how is it different from periodontal disease around natural teeth?
Peri-implantitis is bacterial infection of the tissues and bone around a dental implant. Unlike periodontal disease around teeth, implants have no periodontal ligament, so bone loss from peri-implantitis can be more severe and faster. It requires aggressive treatment to preserve the implant.
Can peri-implantitis be cured, or will my implant eventually need to be removed?
Early peri-implantitis responds well to treatment. Bone loss can be arrested and sometimes reversed with deep cleaning, antibiotics, and improved hygiene. Advanced cases with severe bone loss may require implant removal. Early detection and aggressive treatment maximize your chances of saving the implant.
If I get peri-implantitis, does that mean my immune system is weak?
Not necessarily. Peri-implantitis is primarily a biofilm problem, not a systemic immune deficiency issue. However, diabetes, smoking, and certain genetic factors do increase susceptibility. We assess your specific risk factors during evaluation.
Will my implant feel loose forever if I have peri-implantitis, or can stability be restored?
Implant stability depends on bone support. Once we eliminate infection and arrest bone loss, the implant becomes stable again. Bone remodeling takes months, so improvement happens gradually. Your implant may feel slightly mobile during the healing phase but stabilizes as bone regenerates.
Do water flossers or special irrigation devices help treat peri-implantitis at home?
Home irrigation can reduce bacterial load and support professional treatment, but it cannot treat established peri-implantitis alone. Home care is essential for maintenance after professional treatment, but active infection requires clinical intervention including scaling and possible surgical therapy.
Related Patient Success Stories
Explore similar patient success stories demonstrating our expertise in advanced prosthetic dentistry.

Temporary Crowns Restore Patient's Smile in Just One Day with an Immediate Smile Makeover
A patient from Potomac, Maryland, came to Elite Prosthetic Dentistry with the chief complaint of pain from a failing dental implant and its significant impact on her appearance.
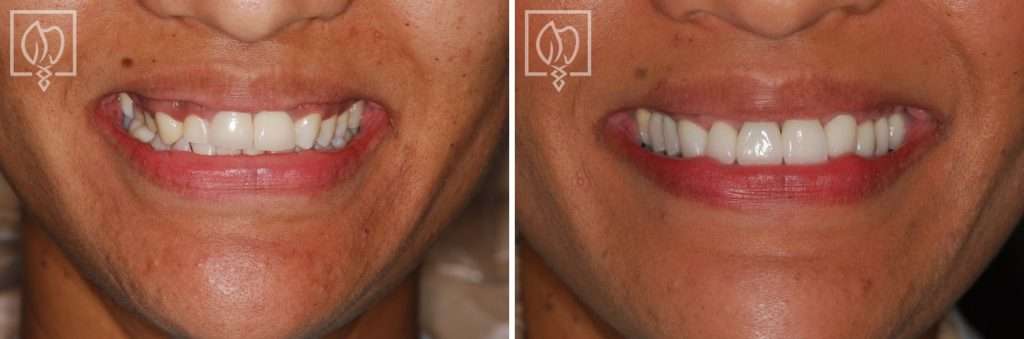
Multi-Faceted Treatment for Patient Unhappy With Her Artificial-Looking Crowns, Teeth and Gums
Many patients come to Elite Prosthetic Dentistry unhappy with the appearance of their smile. However, this particular patient presented with multiple interconnected problems that together created a smile she found deeply unsatisfying.

Treating Kevin’s Collapsed Bite with a Complete Smile Makeover with New Dentures
Dentures are sometimes not created to the ideal aesthetic and functional scheme. When improperly fabricated, dentures can make an individual appear almost a generation older than their actual age. They can have a poor fit that feels loose and unstable when eating or speaking, and they can actually accelerate bone loss over time.

Salvaging Ms. N’s Severely Broken-Down Upper and Lower Teeth from Gum and Bone Disease
Many people in the U.S. suffer from extensive periodontal disease characterized by significant bone loss and shrinkage of the gum tissue. This condition can begin at a very young age and worsen quickly due to hereditary factors and lack of early diagnosis by their dentist.

Rejuvenating Maria’s Severely Worn Down Implant Overdentures
Many times, per year, patients come to us frustrated because their implant prosthesis is so severely worn down that they are very self-conscious and cover up their smile. They look and feel much older than their age as a result of the extensive wear of their appliance(s).
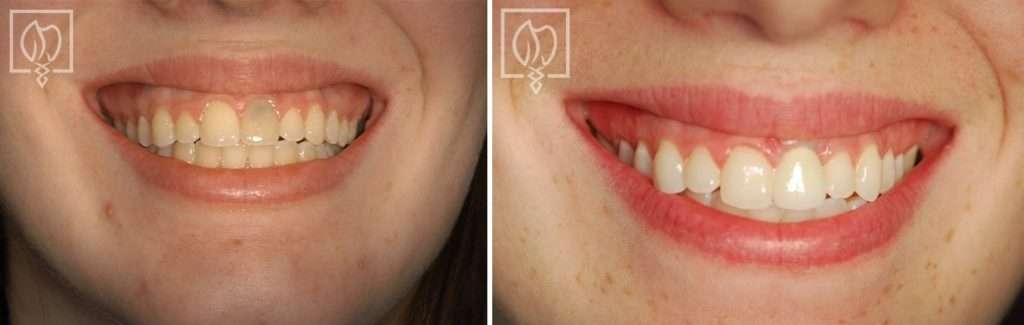
Replacing a Discolored Front Tooth with a Precision Placed Implant
Some of the most challenging restorations occur when fabricating an anterior crown to fit on an implant. Not only does one have the difficulty of matching the single front tooth to the other ones in the high visibility zone, but the dentist must also ensure the position of the underlying implant is precise through accurate preplanning and placement.
Related Articles
Deepen your knowledge with additional insights on this topic.
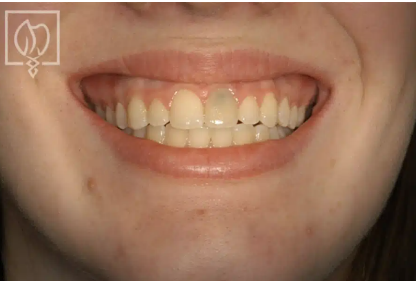 Dental Implants
Dental Implants If a Single Front Tooth is Replaced with an Implant, can it Look Natural?
A single front tooth implant can look completely natural with precision placement, custom abutments, and hand-crafted porcelain crowns. Washington, DC.
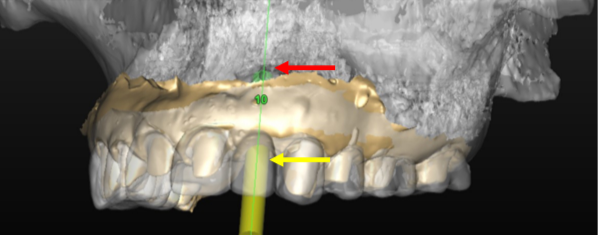 Dental Implants
Dental Implants What is Precision Implant Placement (PIP)?
Learn what Precision Implant Placement (PIP) is and how meticulous planning ensures optimal implant positioning for long-lasting results in Washington, DC.
 Dental Implants
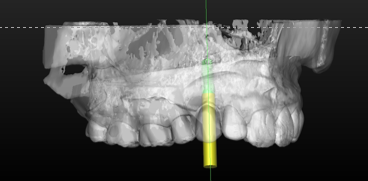
Dental Implants What is the ideal Surgical Guide for Precision Implant Placement?
CBCT-based surgical guides allow virtual implant planning for precise positioning in optimal bone, ensuring predictable results in Washington, DC.
 Dental Implants
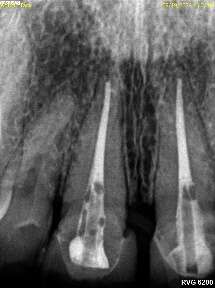
Dental Implants When Should an Implant not be Done?
Not every patient is a candidate for dental implants. Learn when healthy roots, fragile bone, or steep angles may make alternatives the better choice.
 Dental Implants
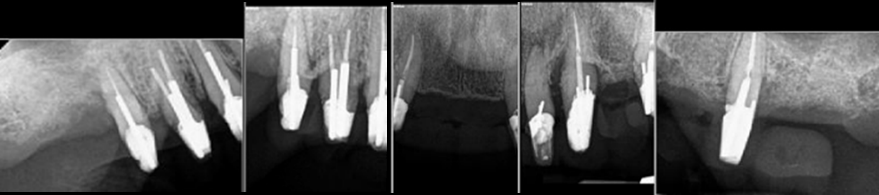
Dental Implants What is Staged Implant Therapy?
Staged implant therapy replaces teeth gradually using existing teeth as temporary support. A personalized alternative to All-on-X for full-arch cases.
Unveiling the Four Types of Dental Implants: Which One's for You?
Learn about the four types of dental implants - endosteal, subperiosteal, zygomatic, and mini implants - and which option may be right for your needs.
Our Services in Chevy Chase
Beyond loose-dental-implant, Chevy Chase patients rely on Dr. Gerald Marlin for a full range of advanced dental care.
More services available in Chevy Chase:
loose-dental-implant Near Chevy Chase
Dr. Gerald Marlin also provides loose-dental-implant services for patients in these neighboring communities.
Getting Here from Chevy Chase
Elite Prosthetic Dentistry is conveniently located near Chevy Chase, MD.
Located near downtown Chevy Chase. Convenient access via Wisconsin Avenue or Connecticut Avenue.
Address:
4400 Jenifer Street NW, Suite 220
Washington, DC 20015
Phone: (202) 244-2101
Schedule ConsultationSchedule Your Consultation from Chevy Chase
Chevy Chase residents trust Dr. Gerald Marlin for precision dental care. With 3,900+ implants placed and 40+ years of experience, your smile is in expert hands.
