
Failed All-on-4 Implants in Chevy Chase, MD
When one implant fails in your All-on-4 system, the entire bridge is at risk. Expert revision and repair in Chevy Chase. Schedule your consultation today.
Failed All-on-4 Implants in Chevy Chase, MD: When One Implant Fails
All-on-4 dentistry is based on a specific engineering principle: four dental implants, when properly positioned, can successfully support and retain a complete arch of teeth. This system has helped thousands of patients restore their smiles and regain function. However, the system is only as strong as its weakest component. When one implant in an All-on-4 system fails, the entire prosthesis is compromised.
We frequently see Chevy Chase patients who come to us with this exact problem. Their All-on-4 was working well for months or years, and then one implant began to fail. The progression is usually insidious at first. A small amount of movement or clicking becomes more pronounced. They notice increased mobility when they bite. Their bite changes slightly. X-rays reveal bone loss around one implant site. Within weeks, the implant has lost sufficient integration that it no longer contributes to supporting the prosthesis.
This situation represents one of the most challenging scenarios in implant dentistry, and it requires careful planning with expertise in repairing failing implants to resolve successfully.
The Biomechanics of Implant Loss in All-on-4
The All-on-4 system works because four implants, when positioned at strategic angles, create a stable platform for the prosthesis. The implants are usually positioned with two in the anterior region facing straight up, and two in the posterior regions angled outward. This geometry, combined with the fixed prosthesis spanning the entire arch, creates sufficient stability and load distribution to function like natural teeth. This approach is part of our precision implant placement philosophy.
This stability is contingent on all four implants working together. When you remove one implant from the system, the geometry falls apart. The remaining three implants must suddenly bear the entire load by themselves. This is not simply a matter of dividing the force by three. The force distribution becomes uneven and concentrated, causing bone loss around the remaining fixtures.
Consider the biomechanics. If your anterior right implant fails, the remaining three implants are now asymmetrically positioned. When you bite down on the right side of your mouth, the two anterior implants on the left side and the left posterior implant experience excessive stress. The right posterior implant, which was originally positioned to help support that right side, is no longer active. The prosthesis begins to rock or tilt toward the failed implant.
This uneven load distribution accelerates bone loss around the remaining implants. The tissues around those implants are experiencing forces they were not designed to withstand. Additionally, the movement and tilting of the prosthesis creates micromotion at the implant-bone interface, which inhibits healing and promotes bone resorption.
Within weeks or months of losing one implant, you may find that the other three implants begin to show bone loss or may themselves become unstable.
Signs That One of Your All-on-4 Implants Is Failing
Early detection of implant failure allows us to intervene before secondary damage occurs to the remaining implants. Learning to recognize the warning signs is important.
The most obvious sign is increasing mobility or movement of your prosthesis. You may notice that your bridge shifts slightly when you bite, or that it feels less stable than it did previously. You might hear a clicking sound when you chew, which represents the prosthesis moving against the implants or the implant abutments moving against the implants themselves.
Another common sign is a change in your bite. If the prosthesis is shifting because one implant is loose, your back teeth may hit at a slightly different angle, creating an asymmetrical bite feeling. You might notice that you are chewing primarily on one side of your mouth to avoid a sensation of instability on the other side.
Pain or discomfort around a specific implant site is always concerning. This may be sharp pain when biting, dull aching, or tenderness to touch. Some patients report a feeling of pressure or heaviness around a particular area.
Swelling, drainage, or any sinus tract around an implant site indicates inflammation or infection around that implant. This is an emergency situation that requires immediate attention.
Perhaps most telling are the X-ray findings. Your dentist may have mentioned new bone loss around one implant when you had recent radiographs. Significant bone loss is a sign that integration is failing and may require bone grafting support.
The Failed Implant Removal Process
Once we confirm that an implant has lost integration, we must address it directly. In some cases, especially if the implant is very loose, it can be removed relatively easily. In other cases, where the implant is still partially integrated, the removal is more involved.
We typically use local anesthesia and sometimes sedation dentistry to make the removal process comfortable. We expose the implant surgically, remove any bone that is integrated around the implant threads, and carefully extract the implant itself. We then thoroughly clean the implant socket to remove any infected or diseased bone.
At this point, we assess the quality and quantity of bone remaining at that site. If bone loss has been significant, we may need to perform bone grafting to rebuild the ridge before placing a new implant. If bone quality is adequate, we can proceed directly to new implant placement as part of our full-mouth reconstruction plan.
Planning Your Replacement Strategy
After removing a failed implant, you face a decision point. What is the best way to restore function and stability to your All-on-4 system?
One option is to replace the failed implant with a new implant in the same location. This returns you to a four-implant system. The advantage of this approach is simplicity and familiarity. Your original prosthesis design was based on four implants, so returning to that configuration makes sense if the bone is adequate.
The disadvantage is that replacing a single implant may not address any underlying problems that caused the original implant to fail. Was the original implant positioned suboptimally? Did it have inadequate primary stability when placed? Did the patient have factors like heavy smoking or diabetes that impaired healing? If the same conditions exist, the new implant may have a similar fate.
Another option is to place two additional implants instead of one, converting your system from All-on-4 to All-on-6. This approach distributes forces more evenly and creates a more robust system overall. If significant bone loss has occurred around the remaining implants, All-on-6 biomechanics may be much safer long-term.
A third option, depending on the location of the failed implant and the integrity of the remaining implants, is to modify your prosthesis to a configuration supported by fewer implants in a different design. This is less common but may be appropriate in specific situations.
Bone Grafting Considerations
Many patients who come to us with a failed All-on-4 implant have experienced substantial bone loss. This bone loss is usually concentrated around the failed implant, but adjacent implants may also show resorption due to the altered loading they experienced while the failed implant was loose.
If bone loss is significant, we may recommend bone grafting before placing a replacement implant. Bone grafting rebuilds the ridge and provides a better foundation for the new implant. We have several options for bone graft material, including autogenous bone from your own body, allogeneic bone from a tissue bank, xenogeneic bone from animal sources, or synthetic bone substitutes.
Our in-house laboratory allows us to prepare bone graft materials and manage the graft placement directly. This gives us greater control over the surgical outcome and allows us to monitor healing closely.
The bone graft typically requires several months of healing before we place a new implant. During this time, your All-on-4 prosthesis remains in place, now supported by three implants. We may need to reinforce the prosthesis or modify it slightly to ensure adequate stability during this interim period.
Timeline for Replacement and Return to Function
Once we have removed a failed implant and assessed the bone, here is the typical timeline for resolution.
If no bone grafting is necessary, we place a new implant at the time of removal. We then allow four to six months for osseointegration. During this time, you continue wearing your three-implant prosthesis, which we may have modified slightly for stability.
After osseointegration is complete, we begin the process of connecting the new implant to your prosthesis. We may need to fabricate a new prosthesis that incorporates the new implant, or we may be able to modify your existing prosthesis if the new implant position is similar to the original.
The full timeline from failed implant removal to final restoration is typically six to nine months.
If bone grafting is needed, the timeline extends. We perform grafting at the time of implant removal, allow six to eight weeks for bone graft incorporation, place a new implant, allow four to six months for osseointegration, and then restore the implant. The total timeline in this scenario is typically nine to fourteen months.
Throughout this process, you remain functional. Your prosthesis, even while supported by fewer implants, continues to allow you to eat and speak. We manage any stability issues through adjustments and modifications as needed.
Prevention of Future Implant Loss
The fact that one implant in your All-on-4 has failed is a setback, but it does not mean you cannot successfully complete a revision that lasts many years. However, understanding why the original implant failed is important so we can avoid repeating that problem.
Common causes of implant failure include inadequate implant position that created excessive stress on that implant, insufficient primary stability at implant placement, bone loss due to uncontrolled gum disease, heavy smoking that impaired healing, or excessive forces due to bruxism or clenching.
During your replacement planning, we address each of these factors. If gum disease was a problem, we establish excellent oral hygiene. If smoking is a factor, we discuss cessation or significant reduction. If bruxism is present, we recommend a protective nightguard.
We also ensure that your replacement implant is placed in optimal position, with adequate bone support and proper primary stability. We use advanced imaging and guided implant placement techniques to maximize the probability of success.
The Specialized Approach to Complex Cases
When one implant in an All-on-4 system fails, you need a specialist who understands the biomechanics, the systemic factors that influence healing, and the surgical techniques required to salvage the situation. General dentists and high-volume implant centers often are not equipped to manage this complex scenario with the care and expertise it requires.
Dr. Gerald Marlin brings two key credentials to your case. He is a prosthodontist, meaning he has specialized training in the design, fabrication, and management of prosthetic restorations. He is also an implant specialist with years of additional training in complex implant cases. This combination of expertise is essential when revision of a failed All-on-4 system is needed.
Additionally, our in-house laboratory means that modifications to your prosthesis can be made quickly and with direct oversight. If your bridge needs adjustment during the healing phases, we do not have to wait for a distant lab. We make the modification ourselves and get you back to full function as quickly as possible.
Serving Chevy Chase with Advanced Care
Chevy Chase residents have high expectations for healthcare quality, and many have experienced the frustration of implant failure elsewhere. When you come to us with a failed All-on-4 implant, we do not rush toward the quickest solution. We take time to understand your situation, explain the factors that led to failure, and propose a comprehensive plan that will work long-term.
We also recognize that implant failure is emotionally difficult. You invested in the original All-on-4 with the expectation that it would work for many years. The fact that it failed is disappointing. We approach your care with empathy while maintaining the objectivity and expertise needed to give you the best possible outcome.
If you are struggling with a failed implant in your All-on-4 system, contact us for a detailed evaluation. We will assess your situation, discuss all options, and create a clear plan forward. Implant failure is not the end of the story. In most cases, successful revision is absolutely possible with the right approach and expertise.
Additional Resources
Learn more about our full-mouth dental implants approach, our repairing failing implants techniques, and our comprehensive bone grafting services. If you need revision work, understand what full-mouth reconstruction failure means and how we address it. Review our in-house laboratory capabilities for custom prosthesis design. Explore Dr. Marlin’s expertise in precision implant placement and visit his biography at meet Dr. Gerald Marlin. Learn about concierge dentistry support through complex cases. We welcome second opinions and are ready to schedule your consultation.
Frequently Asked Questions
What happens if one of my four implants fails in an All-on-4 system?
When one implant loses integration or becomes compromised, the entire All-on-4 prosthesis loses stability and support. The remaining three implants must suddenly carry the full load, creating uneven forces and accelerating bone loss around those implants. The prosthesis often becomes loose and unstable.
Can a single failed implant in All-on-4 be replaced while keeping the prosthesis?
In some cases, we can place a new implant adjacent to or in place of the failed one, but the existing prosthesis usually needs to be redesigned or replaced to accommodate the new implant position. A simple repair is rarely possible.
How do I know if one of my All-on-4 implants is failing?
Signs include increasing mobility or movement of your prosthesis, clicking or shifting when you bite or speak, new bone loss visible on X-rays, pain or discomfort around a specific implant site, or drainage or swelling near one of the implant locations.
Is converting to All-on-5 or All-on-6 better than replacing a single failed implant?
Adding an implant to create All-on-5 or All-on-6 distributes forces more evenly and is often biomechanically superior to a three-implant system. If bone loss is significant, additional implants may be the most reliable solution long-term.
How long does it take to replace a failed implant in an All-on-4 system?
The timeline depends on whether the failed implant needs to be removed and whether bone grafting is necessary. Generally, remove the failed implant, allow healing for several months, place a new implant, and then wait for osseointegration before fitting a new or modified prosthesis. The total process typically takes four to six months.
Related Patient Success Stories
Explore similar patient success stories demonstrating our expertise in advanced prosthetic dentistry.

Temporary Crowns Restore Patient's Smile in Just One Day with an Immediate Smile Makeover
A patient from Potomac, Maryland, came to Elite Prosthetic Dentistry with the chief complaint of pain from a failing dental implant and its significant impact on her appearance.
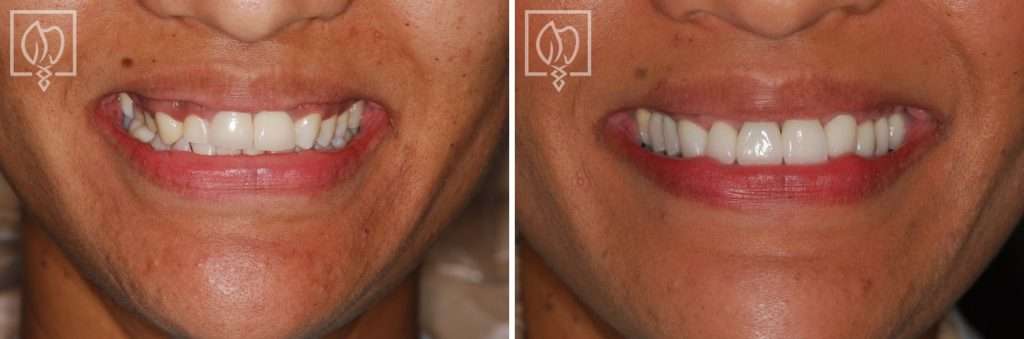
Multi-Faceted Treatment for Patient Unhappy With Her Artificial-Looking Crowns, Teeth and Gums
Many patients come to Elite Prosthetic Dentistry unhappy with the appearance of their smile. However, this particular patient presented with multiple interconnected problems that together created a smile she found deeply unsatisfying.

Treating Kevin’s Collapsed Bite with a Complete Smile Makeover with New Dentures
Dentures are sometimes not created to the ideal aesthetic and functional scheme. When improperly fabricated, dentures can make an individual appear almost a generation older than their actual age. They can have a poor fit that feels loose and unstable when eating or speaking, and they can actually accelerate bone loss over time.

Salvaging Ms. N’s Severely Broken-Down Upper and Lower Teeth from Gum and Bone Disease
Many people in the U.S. suffer from extensive periodontal disease characterized by significant bone loss and shrinkage of the gum tissue. This condition can begin at a very young age and worsen quickly due to hereditary factors and lack of early diagnosis by their dentist.

Rejuvenating Maria’s Severely Worn Down Implant Overdentures
Many times, per year, patients come to us frustrated because their implant prosthesis is so severely worn down that they are very self-conscious and cover up their smile. They look and feel much older than their age as a result of the extensive wear of their appliance(s).
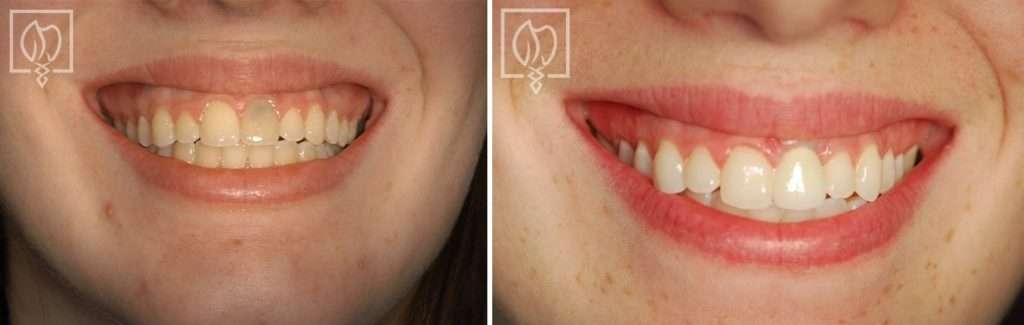
Replacing a Discolored Front Tooth with a Precision Placed Implant
Some of the most challenging restorations occur when fabricating an anterior crown to fit on an implant. Not only does one have the difficulty of matching the single front tooth to the other ones in the high visibility zone, but the dentist must also ensure the position of the underlying implant is precise through accurate preplanning and placement.
Related Articles
Deepen your knowledge with additional insights on this topic.
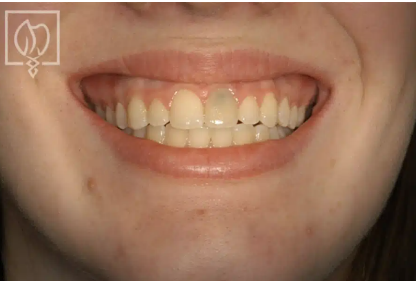 Dental Implants
Dental Implants If a Single Front Tooth is Replaced with an Implant, can it Look Natural?
A single front tooth implant can look completely natural with precision placement, custom abutments, and hand-crafted porcelain crowns. Washington, DC.
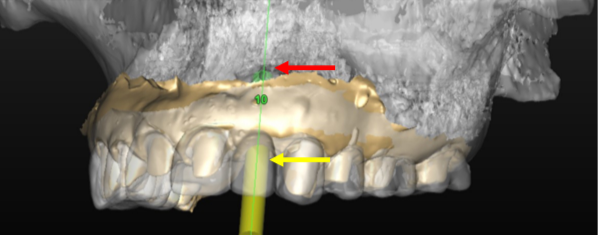 Dental Implants
Dental Implants What is Precision Implant Placement (PIP)?
Learn what Precision Implant Placement (PIP) is and how meticulous planning ensures optimal implant positioning for long-lasting results in Washington, DC.
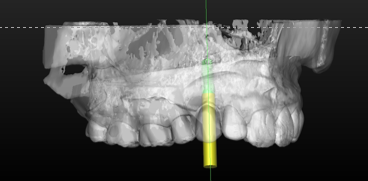 Dental Implants
Dental Implants What is the ideal Surgical Guide for Precision Implant Placement?
CBCT-based surgical guides allow virtual implant planning for precise positioning in optimal bone, ensuring predictable results in Washington, DC.
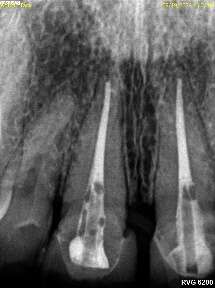 Dental Implants
Dental Implants When Should an Implant not be Done?
Not every patient is a candidate for dental implants. Learn when healthy roots, fragile bone, or steep angles may make alternatives the better choice.
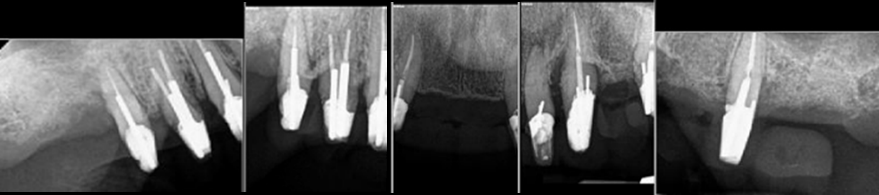 Dental Implants
Dental Implants What is Staged Implant Therapy?
Staged implant therapy replaces teeth gradually using existing teeth as temporary support. A personalized alternative to All-on-X for full-arch cases.
Unveiling the Four Types of Dental Implants: Which One's for You?
Learn about the four types of dental implants - endosteal, subperiosteal, zygomatic, and mini implants - and which option may be right for your needs.
Our Services in Chevy Chase
Beyond failed-all-on-4, Chevy Chase patients rely on Dr. Gerald Marlin for a full range of advanced dental care.
More services available in Chevy Chase:
failed-all-on-4 Near Chevy Chase
Dr. Gerald Marlin also provides failed-all-on-4 services for patients in these neighboring communities.
Getting Here from Chevy Chase
Elite Prosthetic Dentistry is conveniently located near Chevy Chase, MD.
Elite Prosthetic Dentistry is just minutes from Chevy Chase, accessible via Connecticut Avenue or Maryland Route 355.
Address:
4400 Jenifer Street NW, Suite 220
Washington, DC 20015
Phone: (202) 244-2101
Schedule ConsultationSchedule Your Consultation from Chevy Chase
Chevy Chase residents trust Dr. Gerald Marlin for precision dental care. With 3,900+ implants placed and 40+ years of experience, your smile is in expert hands.
