
Loose Dental Implant in Great Falls, VA
Should we save your failing implant or replace it? Dr. Marlin evaluates salvage vs replacement with systematic decision-making. Great Falls prosthodontist.
Loose Dental Implant: Salvage vs. Replacement Decision-Making in Great Falls, VA
When an implant becomes loose and compromised, you face a pivotal decision: should we attempt to save the implant through focused treatment, or should we plan for removal and replacement with a fresh start? This decision is not always obvious, and it depends on many factors unique to your situation. At Elite Prosthetic Dentistry, we systematically evaluate both options, discuss the trade-offs clearly, and help you make the decision that’s right for your specific circumstances.
The Salvage vs. Replacement Framework
Before we can discuss which path makes sense for your implant, let’s understand what each approach entails and when each is most appropriate.
The Salvage Approach
Salvage means we attempt to arrest the problem, stabilize the implant, and preserve the existing fixture. This approach values the implant investment you’ve already made and aims to keep the fixture in place.
Salvage is appropriate when:
- The underlying cause is identifiable and treatable
- Bone loss is moderate, not severe
- No signs of persistent infection
- The implant placement quality is reasonable
- The patient prefers to preserve the fixture
The Replacement Approach
Replacement means we remove the compromised implant and place a new one in optimal position using precision implant placement techniques. This approach prioritizes long-term stability and function over preserving the existing fixture.
Replacement is appropriate when:
- Bone loss is severe (more than half the implant length)
- Persistent infection despite salvage attempts (requiring peri-implantitis treatment)
- Implant placement is fundamentally poor, causing mechanical problems
- The patient values optimization over salvage
- Multiple complications exist simultaneously, including bone loss and positioning issues
The Hybrid Approach
Sometimes we attempt salvage with a clear timeline and exit criteria. If the implant stabilizes over a reasonable period, we’ve succeeded. If it continues to loosen despite intervention, we transition to replacement.
This approach honors both perspectives: we try to save the implant, but we don’t commit indefinitely to a failing cause.
Evaluating Your Implant for Salvage Potential
Determining whether your implant is a good salvage candidate involves systematic assessment.
Assessing Bone Loss Severity
Radiographic Measurement
We measure the amount of bone loss around your implant on radiographs. We compare original implant placement radiographs to current images when available.
Bone loss is expressed as a percentage of the implant length. Minimal bone loss (less than 2-3 mm) represents a salvageable situation. Moderate bone loss (5-7 mm) can sometimes be salvaged but requires aggressive treatment. Severe bone loss (more than half the implant length) generally indicates replacement is more appropriate.
Progression Rate
We assess how quickly the bone loss is occurring. Bone loss that occurs over years suggests a chronic problem that might be stabilized. Rapid bone loss over weeks or months suggests an acute problem (active infection) that requires urgent intervention.
Identifying the Underlying Cause
Infection Assessment
We assess whether active peri-implantitis is present. Signs include redness, swelling, drainage, bleeding with probing, or pus expression.
Active infection that’s unresponsive to treatment is a bad prognostic sign for salvage. Patients with resistant infections often do better with implant removal and replacement.
If infection is present but mild and responsive to antibiotic therapy, salvage becomes more viable.
Force and Biomechanics Assessment
We assess your bite and oral habits. Is overloading contributing? Do we have evidence of grinding or clenching?
If overloading is the problem, addressing it (nightguard, diet modification, bite adjustment) can allow the implant to stabilize.
Position Quality Assessment
Is the implant positioned reasonably well? Or is placement fundamentally poor with severe angulation or depth problems?
Well-positioned implants with bone loss from other causes (infection, overloading) have better salvage prospects than poorly positioned implants.
Medical Factor Assessment
Do you have medical conditions or medications that impaired initial healing and might limit salvage success? (Diabetes, immunosuppression, radiation therapy, bisphosphonates)
If salvageable medical factors exist, addressing them might improve implant stability.
Patient Preference and Values
Time and Convenience
Salvage attempts might require multiple appointments over weeks or months. Replacement is a more defined timeline. Discuss your preference.
Cost Considerations
Salvage attempts might fail, requiring subsequent replacement and thus more total cost. Replacement is definitive but requires implant and restoration cost.
Implant Value Perspective
Some patients strongly prefer to preserve the existing implant, seeing it as an investment worth saving. Others prefer optimization and fresh-start replacement even if it means losing the existing fixture.
Both perspectives are valid. Our role is to inform you about which approach makes sense given your clinical situation, then support your values-based decision.
Salvage Treatment Protocols
If you and Dr. Marlin decide to attempt salvage, here’s what that typically involves.
Non-Surgical Salvage Phase
Infection Treatment
If peri-implantitis is present, we treat aggressively:
- Mechanical removal of biofilm through professional scaling
- Prescription antibiotics (typically amoxicillin plus metronidazole for 7-10 days)
- Antimicrobial rinses (chlorhexidine) during healing
- Enhanced home care instruction
- Medical optimization (diabetes control, smoking cessation)
Force Modification
We address overloading through:
- Custom nightguard fabrication if grinding is present
- Dietary modification to avoid hard foods
- Bite adjustment to distribute forces more evenly
- Discussion of parafunctional habit awareness
Monitoring Protocol
We schedule follow-up appointments at 2 weeks, 4 weeks, and 8 weeks to assess response.
If clinical signs improve (reduced swelling, reduced drainage, stable mobility), salvage is working.
If signs worsen or remain unchanged despite intervention, we escalate to surgical salvage or recommend replacement.
Surgical Salvage Phase
If non-surgical salvage doesn’t arrest the problem, we consider surgical intervention.
Access Flap Surgery
We create an incision to directly visualize the implant and surrounding bone.
We remove biofilm and calculus from the implant surface with specialized instruments.
We may use implantoplasty (smoothing the exposed implant surface) to reduce bacterial colonization.
Bone Assessment
Surgical access allows us to directly assess bone quantity and quality around the implant.
If bone is completely absent, salvage becomes impossible. If some bone remains, we continue salvage.
Bone Regeneration
If bone defects are present, we place bone graft material to regenerate lost bone.
We might use guided bone regeneration (barrier membranes) to direct bone healing.
We might use growth factors to enhance bone regeneration.
Soft Tissue Graft
If soft tissue has been destroyed by infection, we sometimes place a graft to restore tissue volume and biological support.
Post-Surgical Protocol
We place you on antibiotics post-operatively and schedule close follow-up at 1 week, 2 weeks, 4 weeks, and 8 weeks.
Healing from surgical salvage takes time. Bone remodeling occurs over 3-6 months.
Salvage Timeline and Transition Point
We typically commit to salvage for 8-12 weeks of active treatment. If the implant is stabilizing during this period (reduced mobility, stable or improving bone levels on radiographs, resolution of infection signs), we continue managing it.
If the implant is continuing to loosen or infection persists despite intervention, we transition to replacement planning.
This timeline respects both the value of salvage and the reality that some implants cannot be saved.
Replacement as the Primary Treatment Option
Some loose implants are better addressed through immediate replacement rather than salvage attempts.
When Replacement Is the Clear Choice
Severe Bone Loss
Implants with bone loss exceeding 50 percent of the implant length are extremely difficult to salvage. The remaining bone is insufficient to support the implant reliably long-term.
Replacement is mechanically and biologically superior in these situations.
Persistent Infection
An implant with peri-implantitis that doesn’t respond to aggressive non-surgical and surgical treatment is a salvage failure. Persistent infection often indicates the bacterial biofilm on the implant surface cannot be eradicated, or the bone defect is too severe to resolve.
Removal eliminates the infected implant and allows the site to heal. A replacement implant placed in healed bone has much better prospects.
Implant Fracture
A fractured implant cannot be salvaged. Removal and replacement is the only option.
Severely Tilted or Displaced Implants
An implant placed at a severely incorrect angle or in the wrong position biomechanically is poorly supported.
Attempting to salvage a fundamentally misplaced implant with years of bone loss often fails. Replacement in better position is more successful.
Multiple Complications
An implant with bone loss plus infection plus poor positioning plus overloading is fighting too many battles simultaneously.
Removal and replacement with attention to all these factors (optimal placement, infection control, force management) is more pragmatic than attempting to salvage a multiply compromised fixture.
Replacement Benefits
Optimization Opportunity
Replacement allows us to use surgical planning to position the new implant optimally.
We can use CBCT-based planning and surgical guides to achieve ideal positioning that was perhaps missed on the first implant.
We can select implant size, diameter, and design based on anatomy, which might differ from the first implant.
Fresh Start Biologically
A new implant in healed bone has superior integration prospects compared to an implant trying to recover from infection or severe bone loss.
Predictable Outcome
Replacement with optimal positioning has a high likelihood of long-term success.
Salvage of multiply compromised implants has uncertain long-term prospects.
Replacement Timeline and Considerations
Healing Period
After removal, we wait 4-8 weeks for initial bone healing.
We might place bone graft material at the time of removal to optimize bone quality for replacement placement.
Replacement Placement
At approximately 6-8 weeks post-removal, we place the replacement implant.
Integration Period
The replacement implant heals and integrates for 4-6 months before restoration.
Total Timeline
From decision to replace through fully restored implant is typically 5-7 months.
The Hybrid Approach: Structured Salvage With Clear Exit Criteria
Many of our patients benefit from a structured salvage attempt with clear decision points.
Initial Plan
We attempt salvage with specific treatment goals and a defined timeline.
Specific Measurements
We identify specific clinical findings to improve (swelling reduction, drainage resolution) and specific radiographic goals (bone loss stabilization).
Decision Timeline
At 8-12 weeks, we reassess. If specific goals are met, we continue management.
If goals are not met, we transition to replacement planning.
Patient Agency
You understand from the start that this is a trial of salvage, not an indefinite commitment.
You have agency in the decision to transition to replacement if salvage isn’t working.
This approach honors both the value of salvage and the reality of failed salvage attempts.
Cost Comparison: Salvage vs. Replacement
Understanding the financial implications helps inform your decision.
Salvage Costs
Non-surgical salvage involves multiple appointments, antibiotics, antimicrobial rinses, and monitoring radiographs. Cost is moderate.
Surgical salvage adds the expense of surgical treatment, bone graft material, and increased post-operative care. Cost is higher.
If salvage fails and is followed by replacement, total cost becomes substantial because you’ve invested in both salvage and replacement.
Replacement Costs
Replacement involves removal surgery, healing period, replacement implant placement, integration period, and restoration (abutment plus crown).
Replacement is a defined cost. There’s no uncertainty about expense because you’re not trying a salvage attempt first.
Financial Perspective
Some patients prefer defined replacement cost over the uncertainty of salvage costs that might ultimately fail and require replacement anyway.
Others prefer to attempt salvage and save the replacement cost if successful.
There’s legitimate financial reasoning on both sides.
Great Falls and the Decision-Making Process
Great Falls residents appreciate sophisticated, evidence-based decision-making. The salvage versus replacement decision is exactly this type of complex choice.
Our Great Falls location (20 minutes from central Great Falls) reflects our commitment to serving Northern Virginia patients with the level of expertise and communication you deserve.
Making Your Decision
To help you decide between salvage and replacement, consider:
1. Your Implant’s Prognosis
Does your implant have good salvage potential (moderate bone loss, treatable cause, good position)?
Or does it have poor salvage potential (severe bone loss, persistent infection, poor position)?
2. Your Values
Do you strongly prefer to preserve the existing implant investment if possible?
Or do you prefer optimization and fresh-start replacement?
3. Your Tolerance for Uncertainty
Can you commit to 8-12 weeks of treatment with the possibility of ultimately needing replacement?
Or would you prefer the certainty of replacement planning?
4. Time and Convenience
Does your schedule accommodate multiple salvage appointments?
Or does the defined timeline of replacement suit you better?
5. Financial Considerations
What’s your financial flexibility if salvage costs are incurred and replacement is subsequently needed?
These questions don’t have right or wrong answers. They reflect your unique situation and preferences.
Dr. Marlin’s Role in Your Decision
We provide you with:
Clear, honest assessment of your implant’s salvage potential
Explanation of salvage protocols and realistic success likelihood
Clear explanation of replacement option and timeline
Support for whatever decision you make
Our role is to inform, not to decide for you. You make the decision that aligns with your values, timeline, and preferences.
Related Services and Treatment Coordination
Your salvage versus replacement decision might involve multiple services. Repairing failing implants encompasses salvage strategies for complex cases. Dental implant bone loss is the underlying problem in many salvage scenarios and requires specialized management.
Bone grafting is often part of both salvage surgery and replacement preparation. For Great Falls patients, we offer dental implants in Great Falls, bone grafting in Great Falls, implant repair in Great Falls, full mouth reconstruction in Great Falls, implant denture repair in Great Falls, sedation dentistry in Great Falls, and full mouth dental implants in Great Falls.
Precision implant placement is relevant if replacement proceeds and ensures optimal outcomes. In-house lab capabilities allow us to fabricate components quickly as treatment progresses.
Advanced restorative dentistry principles guide restoration design for salvaged or replaced implants. Second opinion dentistry is available if you want another perspective on salvage versus replacement recommendations.
Scheduling Your Consultation
The salvage versus replacement decision should be made with complete information and careful consideration.
Request an appointment for comprehensive evaluation. Bring any prior records and radiographs related to your implant.
Read more about Dr. Marlin’s approach to complex implant decision-making.
Your loose implant presents a decision point. Salvage preserves what exists but carries uncertain outcomes. Replacement optimizes your situation but requires commitment to a longer timeline. Both are valid paths. We’ll help you understand your specific situation and make the decision that’s right for you.
Frequently Asked Questions
How do you decide whether to try to save a failing implant versus removing and replacing it?
We assess bone loss severity, underlying cause, infection status, position quality, and patient preference. Mild problems with good bone anatomy often justify salvage attempts. Severe bone loss, persistent infection, or poor positioning often favor replacement. We discuss both options and let you decide after understanding the risks and benefits of each.
Is it always worth trying to save a loose implant, or are some cases better addressed with immediate replacement?
Some cases favor replacement over salvage. Severe bone loss (more than 50 percent of implant length), persistent infection despite treatment, poor implant position, or patient preference for optimization might make replacement the better choice. We help you weigh the trade-offs of salvage versus replacement.
If we try to salvage my implant and it fails, can we still replace it?
Yes. If salvage treatment doesn't stabilize the implant, we remove it and proceed with replacement. The salvage attempt hasn't compromised future replacement. We simply transition to plan B.
Does salvage require more appointments and longer treatment than removal and replacement?
Sometimes. Salvage attempts might include multiple treatment appointments (debridement, antimicrobial therapy, surgical intervention) before we know if the implant will stabilize. If salvage fails, we then proceed with removal and replacement, adding total time. Replacement alone might be more time-efficient if salvage success likelihood is low.
Will a salvaged implant be as stable long-term as a newly replaced implant?
It depends on the salvage success and the underlying cause. If salvage arrests bone loss and the implant stabilizes, the long-term prognosis can be excellent. If the underlying cause (heavy grinding, peri-implantitis, poor positioning) is not addressed, the salvaged implant might have ongoing problems. A well-positioned replacement implant, without the history of problems, often has superior long-term outlook.
Related Patient Success Stories
Explore similar patient success stories demonstrating our expertise in advanced prosthetic dentistry.

Temporary Crowns Restore Patient's Smile in Just One Day with an Immediate Smile Makeover
A patient from Potomac, Maryland, came to Elite Prosthetic Dentistry with the chief complaint of pain from a failing dental implant and its significant impact on her appearance.
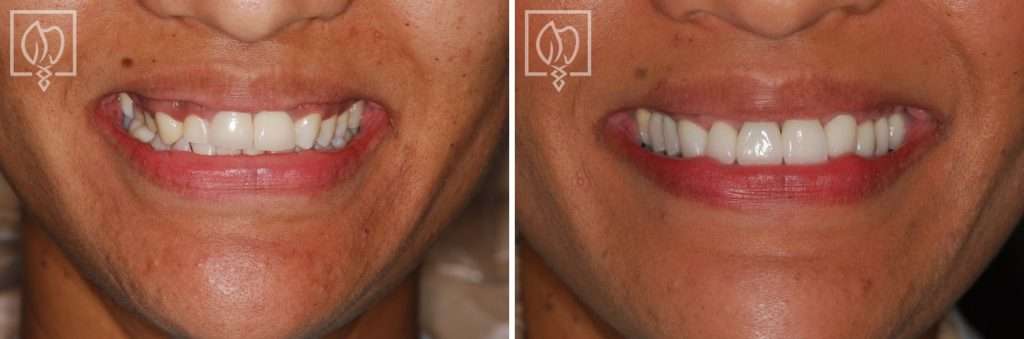
Multi-Faceted Treatment for Patient Unhappy With Her Artificial-Looking Crowns, Teeth and Gums
Many patients come to Elite Prosthetic Dentistry unhappy with the appearance of their smile. However, this particular patient presented with multiple interconnected problems that together created a smile she found deeply unsatisfying.

Treating Kevin’s Collapsed Bite with a Complete Smile Makeover with New Dentures
Dentures are sometimes not created to the ideal aesthetic and functional scheme. When improperly fabricated, dentures can make an individual appear almost a generation older than their actual age. They can have a poor fit that feels loose and unstable when eating or speaking, and they can actually accelerate bone loss over time.

Salvaging Ms. N’s Severely Broken-Down Upper and Lower Teeth from Gum and Bone Disease
Many people in the U.S. suffer from extensive periodontal disease characterized by significant bone loss and shrinkage of the gum tissue. This condition can begin at a very young age and worsen quickly due to hereditary factors and lack of early diagnosis by their dentist.

Rejuvenating Maria’s Severely Worn Down Implant Overdentures
Many times, per year, patients come to us frustrated because their implant prosthesis is so severely worn down that they are very self-conscious and cover up their smile. They look and feel much older than their age as a result of the extensive wear of their appliance(s).
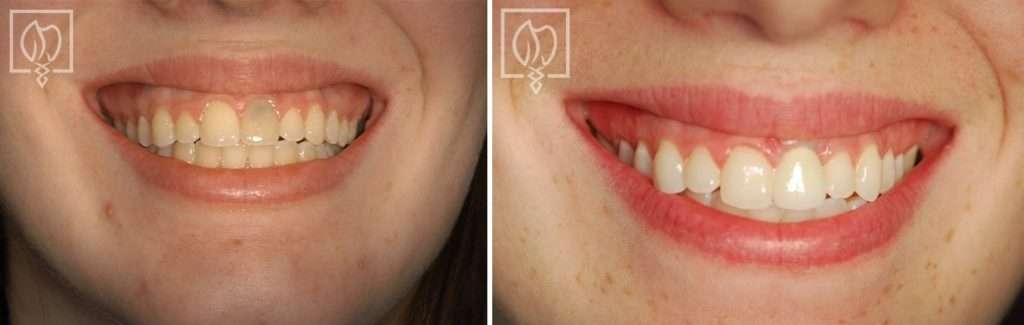
Replacing a Discolored Front Tooth with a Precision Placed Implant
Some of the most challenging restorations occur when fabricating an anterior crown to fit on an implant. Not only does one have the difficulty of matching the single front tooth to the other ones in the high visibility zone, but the dentist must also ensure the position of the underlying implant is precise through accurate preplanning and placement.
Related Articles
Deepen your knowledge with additional insights on this topic.
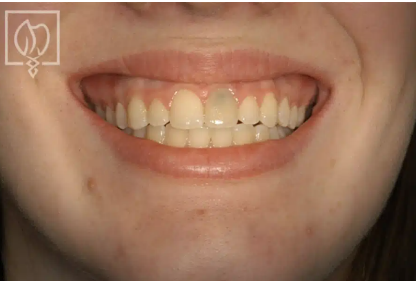 Dental Implants
Dental Implants If a Single Front Tooth is Replaced with an Implant, can it Look Natural?
A single front tooth implant can look completely natural with precision placement, custom abutments, and hand-crafted porcelain crowns. Washington, DC.
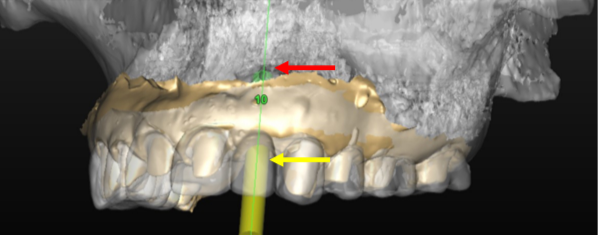 Dental Implants
Dental Implants What is Precision Implant Placement (PIP)?
Learn what Precision Implant Placement (PIP) is and how meticulous planning ensures optimal implant positioning for long-lasting results in Washington, DC.
 Dental Implants
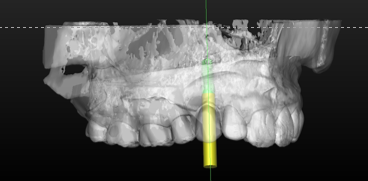
Dental Implants What is the ideal Surgical Guide for Precision Implant Placement?
CBCT-based surgical guides allow virtual implant planning for precise positioning in optimal bone, ensuring predictable results in Washington, DC.
 Dental Implants
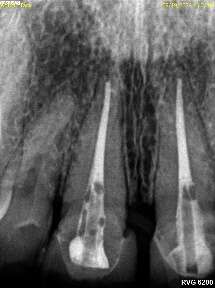
Dental Implants When Should an Implant not be Done?
Not every patient is a candidate for dental implants. Learn when healthy roots, fragile bone, or steep angles may make alternatives the better choice.
 Dental Implants
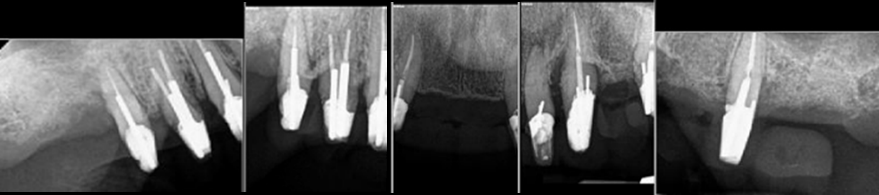
Dental Implants What is Staged Implant Therapy?
Staged implant therapy replaces teeth gradually using existing teeth as temporary support. A personalized alternative to All-on-X for full-arch cases.
Unveiling the Four Types of Dental Implants: Which One's for You?
Learn about the four types of dental implants - endosteal, subperiosteal, zygomatic, and mini implants - and which option may be right for your needs.
Our Services in Great Falls
Beyond loose-dental-implant, Great Falls patients rely on Dr. Gerald Marlin for a full range of advanced dental care.
More services available in Great Falls:
loose-dental-implant Near Great Falls
Dr. Gerald Marlin also provides loose-dental-implant services for patients in these neighboring communities.
Getting Here from Great Falls
Elite Prosthetic Dentistry is conveniently located near Great Falls, VA.
Great Falls is accessible via Route 7 or the Dulles Toll Road. Located northwest of our main office in Fairfax County.
Address:
4400 Jenifer Street NW, Suite 220
Washington, DC 20015
Phone: (202) 244-2101
Schedule ConsultationSchedule Your Consultation from Great Falls
Great Falls residents trust Dr. Gerald Marlin for precision dental care. With 3,900+ implants placed and 40+ years of experience, your smile is in expert hands.
