
Why Veneers Fail: Causes, Warning Signs, and Specialist Solutions
Prosthodontist guide to veneer failure: why veneers break, stain, or debond. Causes, prevention, and expert repair options in Washington DC.
Why Veneers Fail: Understanding the Root Causes
Porcelain veneers represent one of the most successful restorative techniques in cosmetic dentistry when placed by experienced practitioners. Yet many patients come to our practice with veneers that have failed, stained, chipped, or fallen off within just a few years of placement. Understanding why veneers fail is critical to both preventing problems and addressing them when they occur.
Veneer failure is not random. Each failure mode has a specific cause rooted in material science, biomechanics, clinical technique, or bite management. A prosthodontist approaches these problems systematically, asking: What went wrong? Why did it go wrong? How do we prevent it next time?
Types of Veneer Failure and What Causes Them
Veneer Debonding (Falling Off)
When a veneer falls off or debonds from the tooth, the failure lies at the bond interface. The glue didn’t stick well enough to hold the restoration against oral forces. This is the most common failure mode we see in patients coming for second opinions.
The primary cause of debonding is contamination of the bonding surface during the original placement. When a tooth is etched with phosphoric acid, the surface becomes slightly demineralized and ready to accept a chemical bond. If saliva, blood, or any moisture contacts that etched surface before the bonding resin is applied, the bond fails. Many dentists underestimate how critical it is to keep the tooth completely dry during bonding, or they don’t use adequate isolation techniques.
Secondarily, improper acid etching or failure to etch for adequate time weakens the mechanical interlock between the bonding agent and tooth structure. The etching process is not optional or adjustable. Thirty seconds of phosphoric acid on enamel is required. Too little time, and the bond is weak.
A third cause of debonding is bonding agent incompatibility with the veneer material. Different porcelain materials have different surface characteristics. Some ceramics bond better with certain adhesives than others. When a prosthodontist controls both the veneer fabrication and the bonding protocol, this mismatch is eliminated.
Bite forces also contribute to debonding, but typically only if the above factors are already compromised. A properly bonded veneer with good cement selection can withstand normal bite forces indefinitely. However, patients who grind or clench their teeth can overload even a good bond, especially if the preparation design doesn’t provide adequate support or if the veneer is very thin.
Veneer Chipping or Fracture
Porcelain is rigid and strong, but it is also brittle. Unlike natural tooth structure, it cannot flex. When a veneer is loaded beyond its fracture strength, it breaks rather than bends.
Thin veneers, especially ultra-thin “no-prep” veneers, are more prone to chipping and fracture than conventionally prepared veneers with adequate thickness. Many general dentists place veneers that are only 0.5mm thick to minimize tooth removal. At this thickness, even moderate bite forces can cause failure.
Bruxism (nocturnal teeth grinding) is the single most common cause of veneer fracture we see. A patient who grinds their teeth can generate bite forces of 1000 pounds per square inch or more. Porcelain cannot safely withstand this. The solution is identification of bruxism through clinical examination and nightguard fabrication. Many general dentists don’t ask the right screening questions and don’t recommend guards until a veneer has already broken.
Occlusal interferences also cause fracture. If a veneer is positioned with an edge-to-edge contact in centric occlusion, or if the veneer receives the first contact in a lateral movement, the forces concentrate on that veneer. Repeated loading fractures the ceramic. Proper preparation and contouring, combined with careful occlusal adjustment before final cementation, prevents this.
Direct impact trauma breaks veneers. A patient falls, hits their mouth on a steering wheel, or takes a blow to the face. This is unavoidable, but the veneer is designed to sacrifice itself to protect the underlying tooth structure. Fortunately, broken veneers can usually be replaced without damage to the tooth.
Veneer Staining and Color Changes
This is where many patients become frustrated. They were promised a bright white smile, and now their veneers are yellowing, browning, or showing dark lines.
True porcelain veneers do not stain. The glaze-fired surface of a high-quality porcelain is inert and will not absorb color. If a porcelain veneer is yellowing, one of three things has happened: the underlying tooth is darkening and showing through (indicating the veneer is too thin), the margin is staining because the cement is discoloring or microleakage is allowing stain to accumulate, or the veneer is actually composite resin, not porcelain, and the patient was misinformed.
Composite veneers absolutely do stain over time. Composite is a polymer-based material that absorbs pigment. Coffee, red wine, tobacco, and chromogenic foods will stain composite within months. The composite surface also loses its polish over time, becoming duller and more porous. Patients with composite veneers need to understand this trade-off.
Margin staining is a significant problem. The line where the veneer meets the tooth often shows a dark gray or brownish color. This occurs when the resin cement at the margin discolors over time, or when decay begins at the margin (microleakage allows bacteria and acid into the gap). Once margin staining begins, polishing typically cannot remove it without abrading the veneer or exposing the tooth margin.
Gum recession is another cause of apparent veneer staining. As the gum recedes, the natural tooth color shows at the gum line, creating the appearance that the veneer has darkened or changed color. This is actually the underlying tooth showing through. The solution involves cosmetic gum treatment or complete veneer replacement with margins placed in a more protected position.
Gaps and Open Margins
Over time, gaps develop between the veneer and the gum line, or between adjacent veneers. These gaps trap food and allow bacteria to accumulate.
Gum recession is the primary cause. The gum tissue recedes from brushing trauma, periodontal disease, or aging. As it recedes, the veneer margin becomes exposed. If the original preparation placed the margin below the gum line, recession exposes a natural tooth that is not covered by the veneer. This creates both an esthetic problem and a cavity risk.
Inadequate contact points between adjacent veneers also create gaps. If the veneer isn’t contoured to create proper embrasure form and contact point, the papilla flattens and a gap develops. Food packs in, the tissue inflames, and the situation worsens.
Loss of the gum papilla (the tip of the gum between teeth) is both a cause and a consequence of gapped veneers. Loss of papilla allows gaps to enlarge. The gap allows food impaction, which drives further tissue loss.
Material Selection and Its Impact on Longevity
Not all porcelain veneers are equal. The material selected profoundly impacts durability, esthetics, and longevity.
Feldspathic Porcelain
Feldspathic porcelain is the traditional material used in veneers for decades. It is tooth-colored and bonds well. However, feldspathic porcelain is the most brittle of the ceramic materials. It is more prone to chipping and fracture under moderate bite forces. It is also more prone to margin chipping and long-term microleakage because it is more porous than newer ceramics.
Many labs still use feldspathic porcelain because it’s less expensive to fabricate. The material is easier to adjust, etch, and fire. For a patient with excellent oral hygiene, minimal bite forces, and strict diet compliance, feldspathic veneers can last many years. For most patients, however, superior materials are available.
Lithium Disilicate and High-Strength Ceramics
Lithium disilicate and similar pressed or milled ceramics are significantly stronger than feldspathic porcelain. These materials can be made thinner while maintaining strength, allowing more conservative tooth preparation. They are more resistant to chipping and fracture.
The crystalline structure of lithium disilicate gives it superior fracture toughness. When stressed, it is less likely to crack completely. It resists margin chipping better than feldspathic porcelain. It has lower porosity and better marginal seal characteristics.
The trade-off is that high-strength ceramics are more technique-sensitive. They must be etched with hydrofluoric acid rather than phosphoric acid, requiring special protocols. Many general dentists are not trained in these techniques. An experienced prosthodontist lab with proper equipment handles this easily.
For patients with bruxism, clenching, or heavy bite forces, lithium disilicate veneers are clearly superior. For patients with good bite control and excellent care compliance, both materials perform well.
Composite Resin Veneers
Composite veneers are made of tooth-colored plastic reinforced with glass fibers. They bond directly to the tooth with the same adhesive system as composite fillings.
The advantages of composite are speed and cost. A composite veneer can be placed in a single appointment without laboratory fabrication. This makes it attractive for patients with tight budgets or time constraints.
The disadvantages are significant. Composite stains within months to years. It is softer than porcelain and more prone to chipping and wear. It discolors at margins more readily than porcelain. It requires regular polishing and sealing to maintain appearance. Long-term, composite veneers typically require replacement every 5-7 years versus 10-15 years or longer for porcelain.
Composite veneers can be appropriate for patients who want to test the esthetic result before committing to porcelain, or for temporary solutions in young patients whose teeth are still erupting. For definitive restorations, porcelain is superior.
Preparation Design Philosophy and Its Consequences
How much tooth structure is removed during veneer preparation significantly impacts success.
Ultra-Conservative (No-Prep) Veneers
Some dentists market “no-prep” or “no-minimal-prep” veneers. Theoretically, minimal tooth removal preserves more healthy tooth structure. In practice, minimal preparation creates many problems.
Without adequate tooth removal, there is minimal surface area for the bonding resin to contact. The veneer sits on a tooth that is largely untouched by the bur. This reduces mechanical retention and increases reliance on the chemical bond alone. If contamination compromises that chemical bond, debonding is likely.
Additionally, minimal preparation often means the veneer is very thin. Thin veneers are more prone to chipping and fracture. They are also more likely to show the underlying tooth color, appearing gray or dark if the natural tooth is not very light.
No-prep veneers can work in ideal circumstances: excellent tooth color, perfect tooth alignment, perfect occlusion, and excellent patient oral hygiene. For most patients, they are a compromise.
Conservative Preparation
Conventional veneer preparation removes tooth structure in a controlled way: light reduction of the facial surface for veneer space, slight reduction of the incisal edge, and preparation of marginal shoulders and line angles that give the restoration mechanical support and allow adequate veneer thickness.
This approach provides multiple advantages: adequate surface area for bonding, space for adequate ceramic thickness, mechanical support in the preparation line angles, and better control of the final shape and contour.
Conservative preparation removes far less tooth structure than a crown would. Typically, 0.5-1mm of facial reduction is adequate. The tooth structure removal is still “conservative” compared to other restorations, but it is engineered for success.
Preventing Veneer Failure: The Prosthodontist’s Approach
Preventing failure requires attention to every step of the treatment process, from diagnosis through delivery and follow-up care.
Diagnostic Examination
Before any tooth is prepared, a thorough examination identifies risk factors. Does the patient have active clenching or grinding? What is their bite pattern? Are there existing occlusal problems? Does the patient have periodontal disease or a history of gum recession?
Patients with signs of bruxism (flattened cusps, wear facets, muscle pain) are counseled about nightguard use. Patients with unstable occlusions are given an occlusal adjustment or orthodontically corrected before veneer placement. Patients with periodontal disease are treated and brought to health first.
Material Selection
The prosthodontist selects veneer material based on the patient’s specific needs. High-strength ceramic for patients with bruxism or heavy forces. Tooth-colored composite only when there is a specific reason. Standard feldspathic porcelain when indicated, or lithium disilicate when maximum durability is desired.
Preparation Design
Preparation is done with a defined protocol, removing just enough tooth structure to accommodate adequate ceramic thickness while respecting biological limits. Margins are prepared in enamel when possible, improving bond strength and longevity.
In-House Laboratory Control
An in-house lab allows the prosthodontist to oversee every step of fabrication. Shade matching is done under proper lighting with the patient present. Thickness is controlled to specification. Occlusion is verified before the veneer ever enters the patient’s mouth. Contact points are carved to perfection. The surface finish is optimized for bonding.
Bonding Protocol
The bonding procedure follows meticulous protocols. Tooth isolation is absolute, using a rubber dam when possible. The etch is applied for the specified time. Rinsing is thorough. The tooth is dried completely. The bonding agent is applied and light-cured. The veneer is tried in for fit and color. The seating cement is carefully applied, and the veneer is seated with controlled pressure. Excess cement is removed before it hardens.
This is where many failures originate. General dentists often skip steps, use inadequate isolation, or rush the process. A prosthodontist performs this procedure with the care and precision it demands.
Occlusal Adjustment
Before the patient leaves the office, the bite is checked carefully. The veneer should have no premature contacts. There should be no edge-to-edge interference. In lateral movements, the veneer should not be the first tooth to contact. Necessary adjustments are made to the veneer or the opposing teeth.
Nightguard Recommendation
For patients with any signs of bruxism or clenching, a custom nightguard is fabricated. This is not optional or negotiable. It is the most important tool for preventing fracture in at-risk patients.
When Can a Veneer Be Repaired Versus Replaced?
When a veneer fails, the question is whether it can be salvaged or must be replaced.
Debonded Veneer: Rebond or Replace?
A debonded veneer can often be rebonded if the veneer is intact and undamaged. The veneer is cleaned, the resin cement is removed from both the veneer and the tooth, the surfaces are re-etched, and the veneer is re-bonded using an improved technique or a more reliable bonding system.
Rebonding works when the tooth preparation is still sound, there is no decay at the margins, and the fit of the veneer is still accurate. If there is any question about margin seal, decay, or veneer fit, replacement is more reliable.
Chipped Veneer: Polish, Composite, or Replace?
A small chip at the edge of a veneer might be polished or filled with composite resin. This is a temporary fix. Eventually the chip returns or expands.
If the chip is large or the veneer is otherwise compromised, replacement is the best solution. A new veneer provides predictable esthetics and longevity.
Stained Veneer: Can It Be Whitened?
Porcelain veneers cannot be bleached. If staining is marginal, the margin can be polished or resealed. If staining is throughout the veneer, replacement is the only option.
Composite veneers can be polished and may improve slightly, but composite staining is essentially permanent. Replacement with composite or conversion to porcelain is the long-term solution.
Expected Lifespan by Material Type
Research and clinical experience give us predictable lifespans:
Feldspathic porcelain veneers: 7-12 years with good care. Some last longer with excellent care and no bruxism. Some fail sooner due to technique issues.
Lithium disilicate and high-strength ceramic veneers: 10-15 years or longer. Many cases reported at 15+ year success rates.
Composite veneers: 5-7 years before discoloration and wear necessitate replacement.
These are not guarantees. Individual cases vary based on technique, bite management, material quality, and patient compliance.
Maintenance Requirements for Long-Term Success
Patients must understand that veneers require ongoing care.
Oral hygiene should be excellent. Plaque accumulation around margins leads to decay and gum problems. Electric toothbrushes and flossing are essential.
Diet matters. Patients with composite veneers must avoid staining foods and beverages. All patients should avoid hard foods and chewing on non-food objects.
Regular dental visits allow early detection of problems. Margins are examined for staining or breakdown. Occlusion is checked for changes. Gum health is monitored.
Nightguards should be worn by all patients with any signs of bruxism.
Professional cleaning and polishing maintains appearance and allows the dentist to check margins and structure.
Why Prosthodontists Achieve Superior Veneer Outcomes
Prosthodontists train specifically in smile design, material science, occlusal biomechanics, and advanced restorative techniques. We understand the science of how veneers fail and how to prevent failure.
An in-house laboratory under prosthodontist supervision eliminates the variability and miscommunication that plagues veneers placed by general dentists. We control every variable.
We do comprehensive occlusal analysis and management. Many veneer failures are driven by bite problems that general dentists never identify.
We select materials strategically, not based on cost. We recommend high-strength ceramics when indicated, not just standard porcelain because it’s standard.
We prepare teeth thoughtfully, with preservation of tooth structure balanced against durability and retention.
We bond with meticulous technique, never rushing, never skipping steps.
We follow patients long-term, monitoring for problems and addressing them proactively before minor issues become major failures.
Conclusion: From Failure to Success
Veneer failure is not inevitable. When you understand the root causes and work with a specialist who does too, the results are predictable and durable.
If you have failing veneers, we can assess why they failed and restore your smile with results designed to last. We offer second opinions for patients with veneer problems, comprehensive treatment planning, and the expertise to achieve the esthetic results you deserve.
Contact Elite Prosthetic Dentistry to schedule a consultation with Dr. Gerald Marlin.
Your Best Smile Is Within Reach
Schedule a consultation with Dr. Gerald Marlin to discuss your treatment options and take the first step toward a healthier, more confident smile.
Frequently Asked Questions
How long do porcelain veneers actually last?
High-quality porcelain veneers fabricated from lithium disilicate or similar advanced ceramics typically last 10-15 years or longer with proper care and bite management. Composite veneers, while less durable, generally last 5-7 years. Longevity depends heavily on material selection, bonding protocol, tooth preparation design, and the patient's bite forces. A prosthodontist with an in-house lab can control these variables better than general practices relying on outside labs.
What causes veneers to fall off?
Veneers debond when bonding integrity fails, most commonly due to contamination during the original bonding procedure (saliva, blood, or moisture on the tooth surface), insufficient acid etching of the tooth structure, or use of incompatible bonding agents for the veneer material. Excessive bite forces, grinding, or clenching can overload the bond line over time. Poor tooth preparation design that doesn't provide adequate retention also increases debonding risk.
Can a veneer that fell off be rebonded?
Many debonded veneers can be successfully rebonded if the veneer is intact and undamaged, and if the bonding surface can be properly cleaned and re-etched. The original tooth surface must be free of decay or margin breakdown. A prosthodontist will assess the veneer fit, the tooth preparation, and the reason for debonding to determine whether rebonding is a reliable long-term solution or whether replacement is advisable.
Why do some veneers chip or crack?
Veneer fractures occur when ceramic material is loaded beyond its strength limits. Common causes include bruxism (teeth grinding), unmanaged clenching forces, occlusal interferences that concentrate stress on one veneer, inadequate veneer thickness from over-aggressive tooth preparation, and direct impact trauma. Manufacturing defects in the ceramic are rare but possible. Nightguard use and occlusal adjustment can prevent most fractures.
Should I replace all my veneers if one fails?
Not necessarily, but a failed veneer is a signal to evaluate adjacent teeth. If one veneer debonded or fractured, the teeth next to it may be experiencing similar forces and could fail soon after. A comprehensive occlusal assessment by a prosthodontist may reveal bite problems that affect multiple veneers. In some cases, replacing just the failed veneer works well; in others, a coordinated replacement of 2-3 teeth prevents sequential failures.
What's the difference between composite and porcelain veneers in terms of durability?
Porcelain veneers are significantly more durable and stain-resistant than composite. Fired ceramics do not absorb color or discolor over time, while composite resins gradually stain and require periodic polishing and sealing. Porcelain is harder and more resistant to chipping, though it can fracture under extreme force. For patients with moderate-to-heavy bite forces or high cosmetic expectations, porcelain is the superior choice despite higher initial cost.
How does an in-house lab improve veneer success?
An in-house laboratory allows the prosthodontist to directly oversee material selection, shade matching, thickness, contour, and finish. The dentist and ceramist communicate in real time about bite concerns, margin placement, and preparation design. This coordination reduces laboratory errors, improves material consistency, and allows custom adjustments before the veneer is seated. Many veneer failures originate from miscommunication or quality inconsistencies in outside labs.
Related Patient Success Stories
Explore similar patient success stories demonstrating our expertise in advanced prosthetic dentistry.

Temporary Crowns Restore Patient's Smile in Just One Day with an Immediate Smile Makeover
A patient from Potomac, Maryland, came to Elite Prosthetic Dentistry with the chief complaint of pain from a failing dental implant and its significant impact on her appearance.
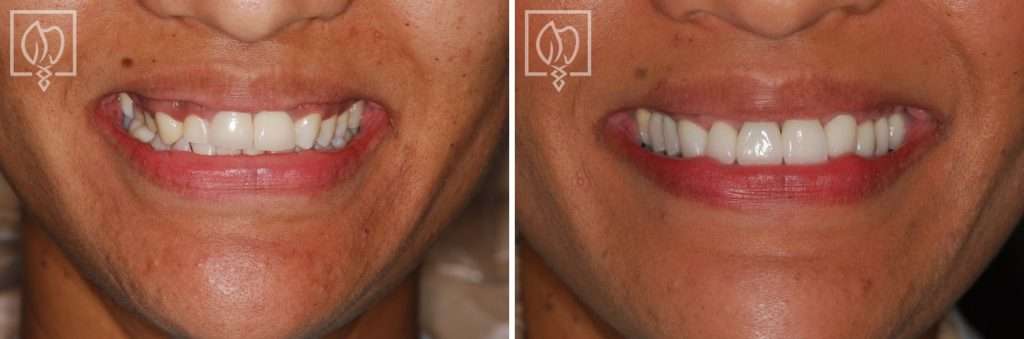
Multi-Faceted Treatment for Patient Unhappy With Her Artificial-Looking Crowns, Teeth and Gums
Many patients come to Elite Prosthetic Dentistry unhappy with the appearance of their smile. However, this particular patient presented with multiple interconnected problems that together created a smile she found deeply unsatisfying.

Treating Kevin’s Collapsed Bite with a Complete Smile Makeover with New Dentures
Dentures are sometimes not created to the ideal aesthetic and functional scheme. When improperly fabricated, dentures can make an individual appear almost a generation older than their actual age. They can have a poor fit that feels loose and unstable when eating or speaking, and they can actually accelerate bone loss over time.

Salvaging Ms. N’s Severely Broken-Down Upper and Lower Teeth from Gum and Bone Disease
Many people in the U.S. suffer from extensive periodontal disease characterized by significant bone loss and shrinkage of the gum tissue. This condition can begin at a very young age and worsen quickly due to hereditary factors and lack of early diagnosis by their dentist.

A Smile Transformation in Just Four Months: A Patient’s Dental Crown Restoration for a TV Series
A patient with dental crowns that were in poor shape was going to appear on a streaming video series on a major TV network that was scheduled to begin filming soon. Our patient, John, an author about to embark on a book tour, was anxious as his teeth were not up to his standards to appear on television.
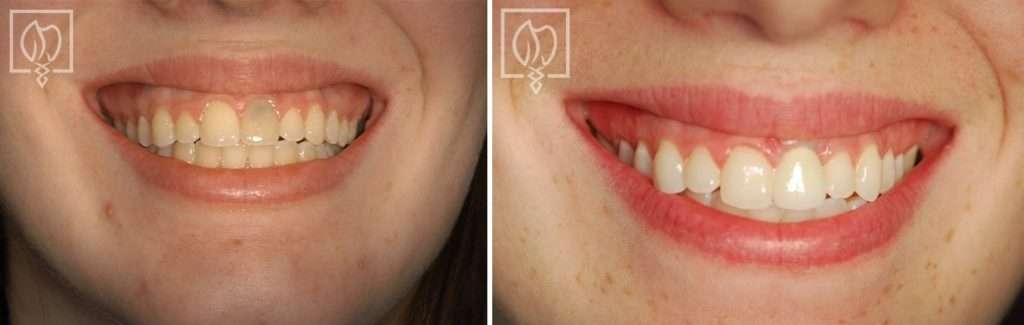
Replacing a Discolored Front Tooth with a Precision Placed Implant
Some of the most challenging restorations occur when fabricating an anterior crown to fit on an implant. Not only does one have the difficulty of matching the single front tooth to the other ones in the high visibility zone, but the dentist must also ensure the position of the underlying implant is precise through accurate preplanning and placement.
Why Veneers Fail: Causes, Warning Signs, and Specialist Solutions Near You
Dr. Gerald Marlin provides why veneers fail: causes, warning signs, and specialist solutions services to patients throughout the Washington, DC metropolitan area. Select your community to learn more.
Ready to Transform Your Smile?
With 40+ years of experience and 3,900+ dental implants placed, Dr. Gerald Marlin delivers results that last. Schedule your consultation today.
