Second Opinion on Failed Dental Implants
A failing implant demands expertise. Our prosthodontist evaluation reveals what went wrong, whether your implant can be saved, and what your best options are moving forward. Not all implant problems require extraction.
Elite Prosthetic Dentistry
Specialist Prosthodontic Practice - 40+ Experience - 3,900+ Implants
97%
Success Rate
3,900+
Implants Placed
40+
Years Specializing
1985
In-House Lab Since

Expert Evaluation You Can Trust
Your failing implant has a history. It was placed by another dentist with specific techniques, materials, and clinical decisions that led to its current condition. To understand what went wrong and whether it can be corrected, you need someone with deep expertise in implant biomechanics and the judgment that comes from evaluating thousands of cases.
Dr. Gerald Marlin brings 40 years of prosthodontic specialization to every failed implant evaluation. He does not rush. He does not assume. He examines thoroughly, images comprehensively, and explains findings clearly so you understand exactly what you are dealing with and what your realistic options are.
When to Seek a Second Opinion on Your Implant
These warning signs warrant a prosthodontist evaluation. Do not assume that implant problems are inevitable or irreversible.
Looseness or Mobility
Movement in an implant tooth indicates a problem that requires diagnosis. The cause may be a loose screw, poor osseointegration, bone loss, or abutment failure. Each requires different treatment. Do not wait to investigate.
Visible Bone Loss on X-rays
Bone loss around an implant visible on radiographs suggests peri-implantitis or mechanical causes. The pattern and severity of bone loss determine whether salvage is possible. Early intervention halts progression.
Recurring Infection
Drainage, swelling, or repeated antibiotics around an implant signal bacterial colonization. Chronic infection damages bone and compromises the implant site. Professional evaluation determines whether infection can be controlled or if the implant must be removed.
Pain That Won't Resolve
Persistent pain around an implant despite treatment suggests undiagnosed problems. Pain may stem from poor bite mechanics, infection, implant fracture, or sinus involvement. A specialist evaluation isolates the cause so treatment can address it specifically.
Aesthetic Problems
A crown that does not match your smile, gum recession, or visible dark lines around an implant may indicate problems with crown design, abutment selection, or bone loss. Many aesthetic failures are correctable through crown replacement or abutment revision.
Implant Placed by Non-Specialist
General dentists place implants without prosthodontic training in bite mechanics and implant biomechanics. Many implants placed by non-specialists fail or develop problems earlier than necessary. A specialist evaluation clarifies whether your implant is sound or at risk.
What Our Evaluation Reveals That Others Miss
A specialist prosthodontist's evaluation differs fundamentally from a general dentist's assessment. We look beyond whether an implant is loose or infected. We analyze the biomechanical systems that support long-term implant success.
Advanced Imaging: CBCT Analysis
Panoramic radiographs show bone height, but CBCT reveals bone density, width, and three-dimensional implant position. We analyze bone loss patterns to distinguish between peri-implantitis (bacterial infection) and mechanical bone loss. We assess proximity to vital structures including the inferior alveolar nerve and maxillary sinus. We evaluate whether an implant is in the correct position relative to adjacent teeth and bite forces. This imaging level is what general dentists typically do not perform.
Bone Quality and Quantity Assessment
Implant success depends on bone support. We assess whether bone loss is localized or systemic, whether the implant threads remain embedded in vital bone, and whether bone regeneration is feasible. Some bone loss is cosmetic only. Other bone loss compromises implant stability. We quantify the difference so you understand your options. Many failing implants can be saved if bone loss is minimal and caught early.
Abutment Connection and Fit
A failing crown often reflects an abutment problem, not an implant problem. We examine the connection between implant and abutment, assess seal integrity, and evaluate whether the abutment is properly seated. A loose abutment screw is correctable. A fractured abutment requires replacement. A poorly fitting abutment causes micromotion and accelerates failure. We diagnose the specific problem so the specific solution is applied.
Occlusal Force Analysis
Implants fail when bite forces exceed the implant's capacity or when forces are directed at harmful angles. We evaluate your bite, identify premature contacts, and assess whether forces are distributed favorably. Some implants fail because the bite is wrong, not because the implant is defective. Correcting the bite often resolves the problem without replacing the implant.
Implant Position Relative to Anatomy
Implants placed at poor angles or locations fail faster and create biomechanical stress. We evaluate whether your implant is positioned to support long-term function and aesthetics. Poor positioning cannot be corrected without removing the implant, but understanding this guides decisions about replacement implant positioning and whether salvage makes sense.
Diagnosis Requires Precision
Clinical examination alone is insufficient. We employ the same advanced diagnostic capabilities used during implant placement: radiographic assessment with CBCT 3D imaging, biomechanical testing, and microbiological analysis when infection is suspected. These tools reveal causes that surface observation misses.
We distinguish between implant failure, component failure, and crown problems. We identify whether bone loss reflects peri-implantitis, mechanical loading, or normal remodeling. We assess whether an implant that feels loose is actually mobile or if it is the abutment connection that is compromised. This precision determines whether your implant can be salvaged.
Once we understand the problem, we present options clearly and discuss which pathway makes sense given your specific situation, your health, and your preferences.
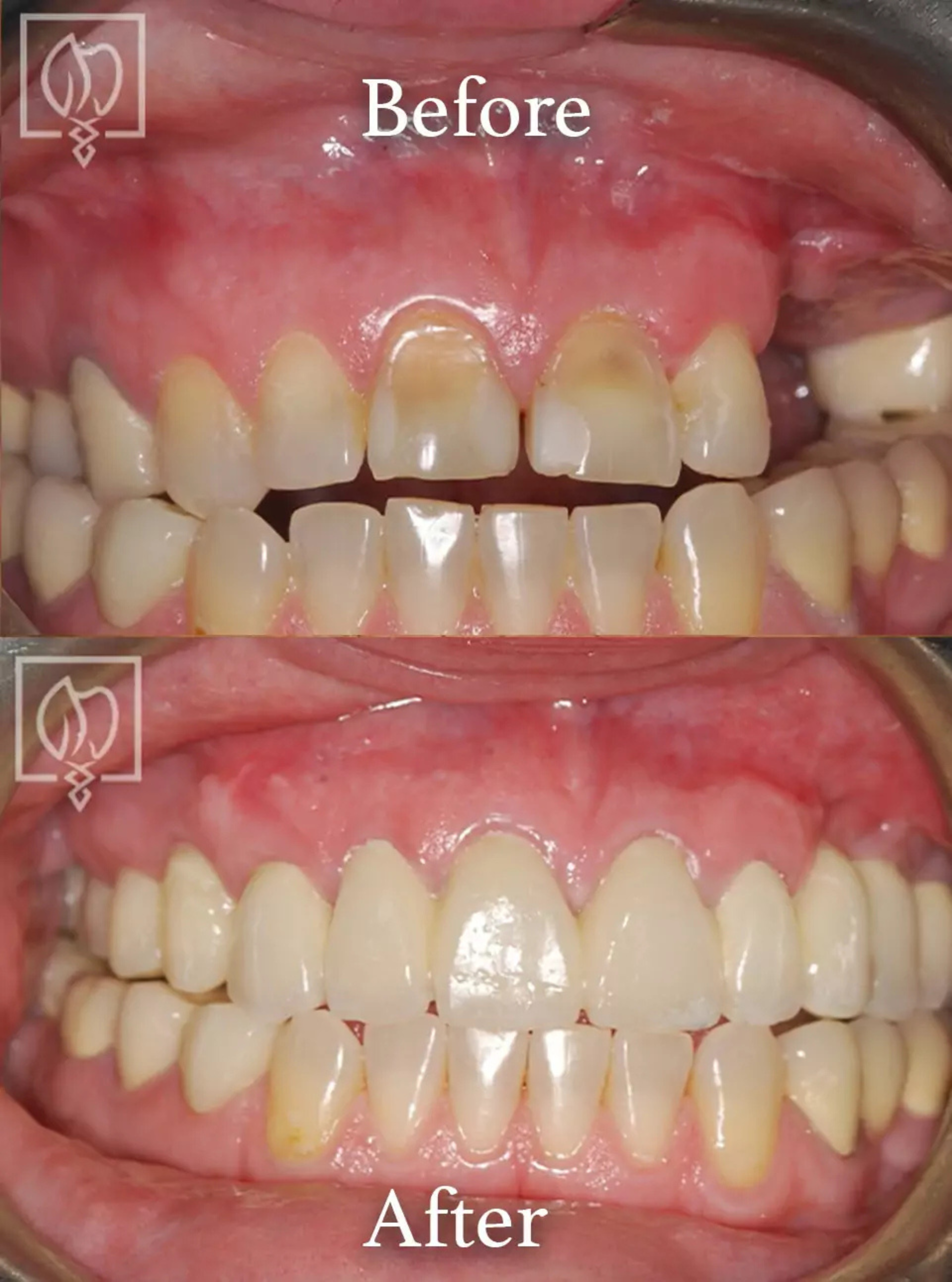
Common Implant Failures We Evaluate
We routinely evaluate these patterns of implant failure. Each has distinct causes, diagnostic pathways, and treatment options.
Loose Dental Implant
An implant that moves or feels unstable may have a loose screw, failed osseointegration, or bone loss. Some loose implants can be salvaged. Others require extraction and replacement.
Learn moreBone Loss Around Implants
Bone loss around an implant indicates infection, poor bite mechanics, or implant failure. We assess severity and determine whether bone regeneration is possible.
Learn morePoorly Placed Implants
Implants placed at wrong angles or locations fail faster and create aesthetic and functional problems. Positioning assessment guides revision treatment.
Learn moreFailed Implant Integration
Osseointegration failure means bone never anchored to the implant. This appears as mobility within weeks to months of placement and requires extraction.
Learn morePeri-Implantitis
Bacterial infection around an implant damages bone and soft tissue. Early treatment can halt progression. Advanced peri-implantitis may require implant removal.
Learn moreImplant Revision
When an implant cannot be salvaged, expert removal and replacement using strategic planning prevents repeat failure.
Learn moreSalvage vs. Replacement: The Decision Framework
After evaluating a failing implant, we determine whether salvage is possible or whether replacement is the best path. This decision rests on multiple factors assessed during your examination.
Bone loss severity drives the decision. Minor localized bone loss (2 to 3 millimeters) around one or two teeth of a multi-rooted implant may be halted through bone regeneration, antimicrobial therapy, and bite correction. We can often save implants with moderate bone loss if the remaining bone is sufficient to support the implant long-term. Advanced bone loss where most threads are exposed and bone surrounds less than 30 percent of the implant makes salvage unlikely. A prosthodontist assesses bone loss using CBCT and determines the threshold where replacement becomes the wise choice.
Implant mobility grade matters. An implant with minimal movement under testing may respond to tightening an abutment screw and correcting the bite. An implant with frank mobility in all directions indicates complete loss of osseointegration and requires removal. The grade of mobility tells us whether the implant ever achieved integration or whether it has since been lost.
The presence and extent of infection influence the decision. Active peri-implantitis with drainage and swelling indicates bacterial colonization. Mild infection may be controlled with antimicrobial therapy, but entrenched, recurrent infection warrants extraction to eliminate the infection source. Cultures and microbial analysis sometimes guide antibiotic selection, but chronic infection resistant to treatment is best resolved by implant removal.
Implant position affects salvage feasibility. An implant at a poor angle may not be salvageable because repositioning is impossible without extraction. An implant in correct position is worth more effort to save. Patient health factors also matter. Your ability to heal, manage oral hygiene, and comply with maintenance affects whether salvage will succeed long-term. A healthier patient with good hygiene is a better candidate for bone regeneration and implant retention.
Cost and time considerations enter the discussion. Salvaging an implant through bone regeneration and correction of bite mechanics takes months and costs less than extracting and replacing it. However, if salvage effort is unlikely to extend the implant's functional life significantly beyond replacement longevity, starting fresh with a properly positioned, properly designed replacement implant is sometimes the strategically sound choice. We present these trade-offs clearly so you can make an informed decision.
Salvage is Often Possible
Many failing implants do not require extraction. When bone loss is moderate and the implant body remains integrated, we can often save it through bone regeneration, correction of bite mechanics, and abutment or crown revision. The implant that was failing becomes stable and functional again.
The decision to salvage or replace depends on multiple factors: the severity and pattern of bone loss, the implant's position relative to your bite, whether infection is present and controllable, and your preference. A specialist evaluation determines where your case falls on this spectrum.
When salvage makes clinical sense, we pursue it thoughtfully. When replacement is the wiser path, we plan the replacement to avoid the mistakes that led to the first failure.
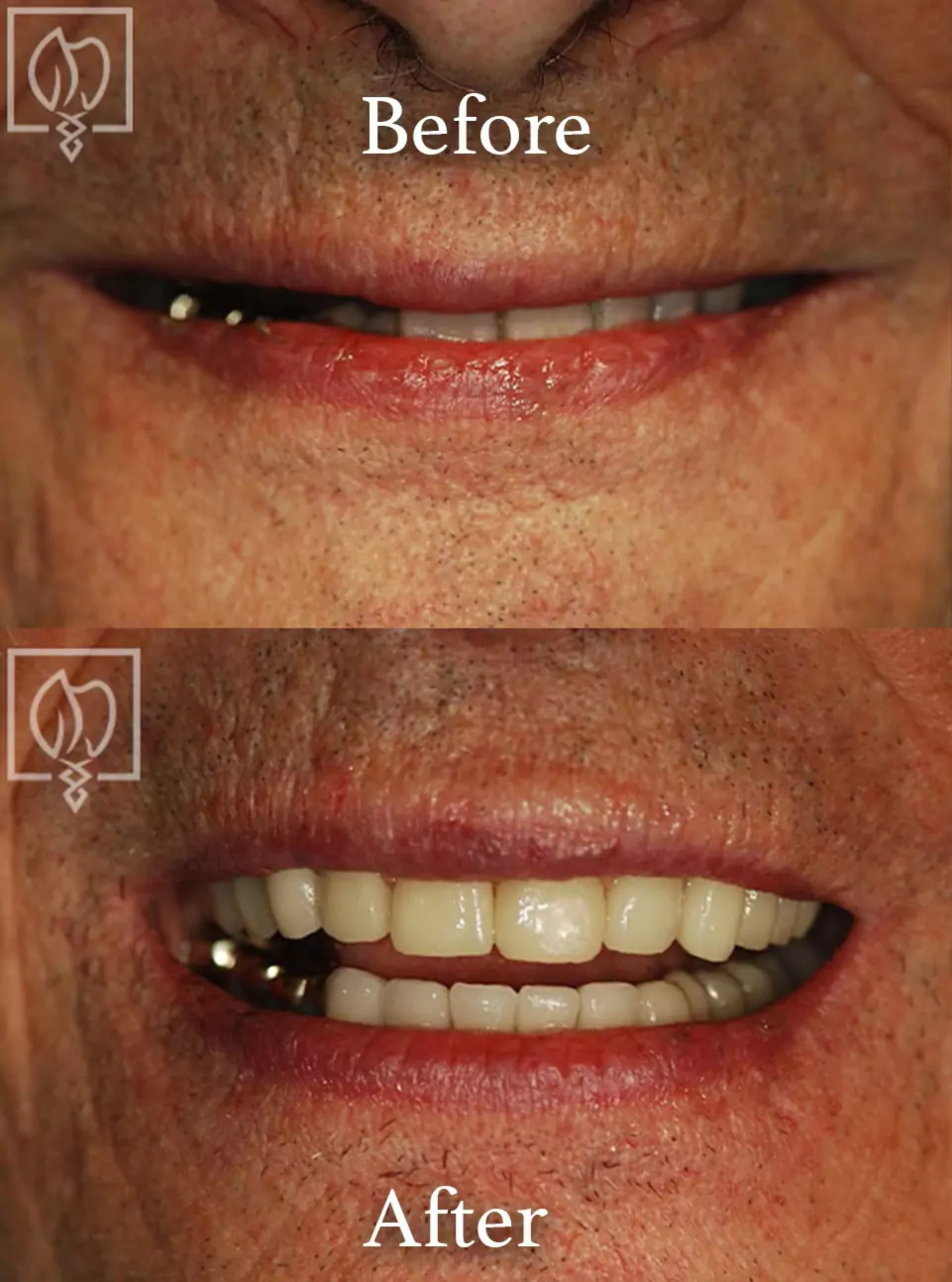
The In-House Laboratory Advantage
Elite's on-site laboratory, in operation since 1985, is integral to managing failed implant cases. When an implant requires abutment revision or crown replacement, we fabricate custom abutments and restorations in-house. This control means we can adjust fit, contour, and screw access immediately during clinical evaluation. We iterate quickly. If a custom abutment does not fit precisely, we modify it before delivery rather than waiting days for external lab revision.
For implant revision cases where the original implant must be removed and replaced, our lab fabricates the final restoration precisely to match your bite and aesthetic requirements. The integration of clinical diagnosis, treatment planning, and fabrication under one roof ensures consistency and precision that off-site labs cannot match.
Learn about our in-house laboratoryFrequently Asked Questions
How do I know if my implant is actually failing?
Can a loose implant always be saved?
What imaging do you use to evaluate failed implants?
My implant was placed by another dentist. Can you evaluate it?
What is peri-implantitis and how do you diagnose it?
How long does a failed implant evaluation take?
What happens after the evaluation?
Your Implant Concern Deserves Expert Evaluation
Do not assume your failing implant is beyond salvage. Many problems respond to specialist intervention. A comprehensive evaluation reveals what is possible.
Specialist prosthodontic evaluation - including advanced imaging and detailed treatment planning - available throughout Washington, DC metro area.
